
U.S. Behavioral Health Market Outlook 2030
Region:North America
Author(s):Shivani Mehra
Product Code:KROD11448
November 2024
97
About the Report
U.S. Behavioral Health Market Overview
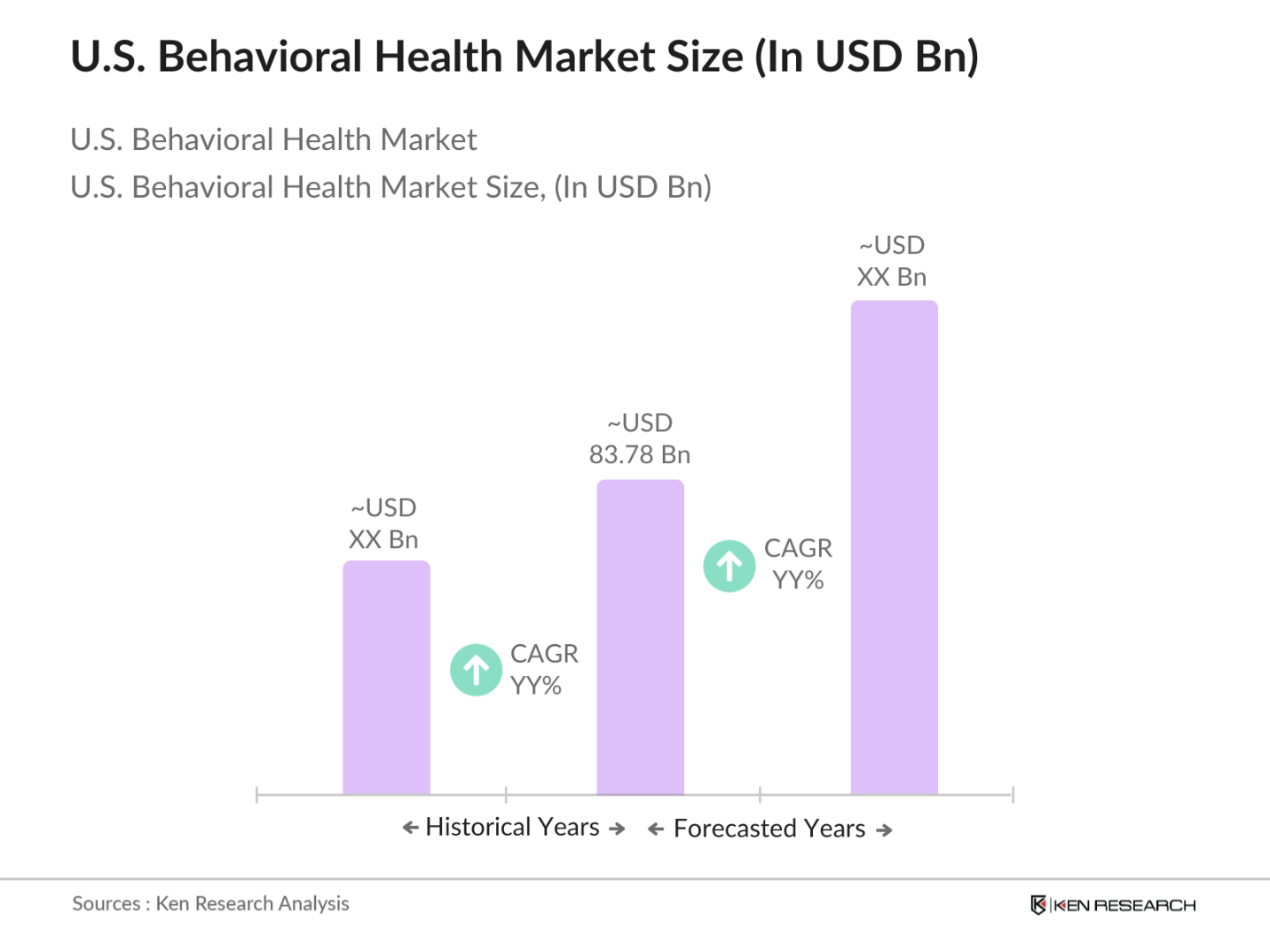
- The U.S. Behavioral Health Market, based on a comprehensive analysis, is valued at approximately USD 83.78 billion. This growth is driven primarily by increased awareness of mental health issues, the expansion of telehealth services, and significant government support through programs such as Medicaid. The demand for services addressing mental health and substance abuse disorders has risen due to societal shifts and the adoption of technology in service delivery.
- Certain U.S. states, including California, New York, and Texas, dominate the behavioral health market. This dominance is due to their large populations, diverse socio-economic structures, and well-established healthcare infrastructures. These regions also benefit from higher state-level funding and support for behavioral health initiatives, driving greater accessibility and use of these services.
- The expansion of Medicaid under the Affordable Care Act (ACA) has been instrumental in increasing access to behavioral health services for low-income individuals. In 2023, Medicaid covered approximately 27 million people for mental health and substance abuse services across the U.S. The federal government has allocated substantial funding to improve mental health service accessibility through Medicaid, allowing more individuals to access treatment for conditions such as depression, anxiety, and substance use disorders. Medicaid now plays a vital role in covering mental health care costs for vulnerable populations, especially in underserved areas.
U.S. Behavioral Health Market Segmentation
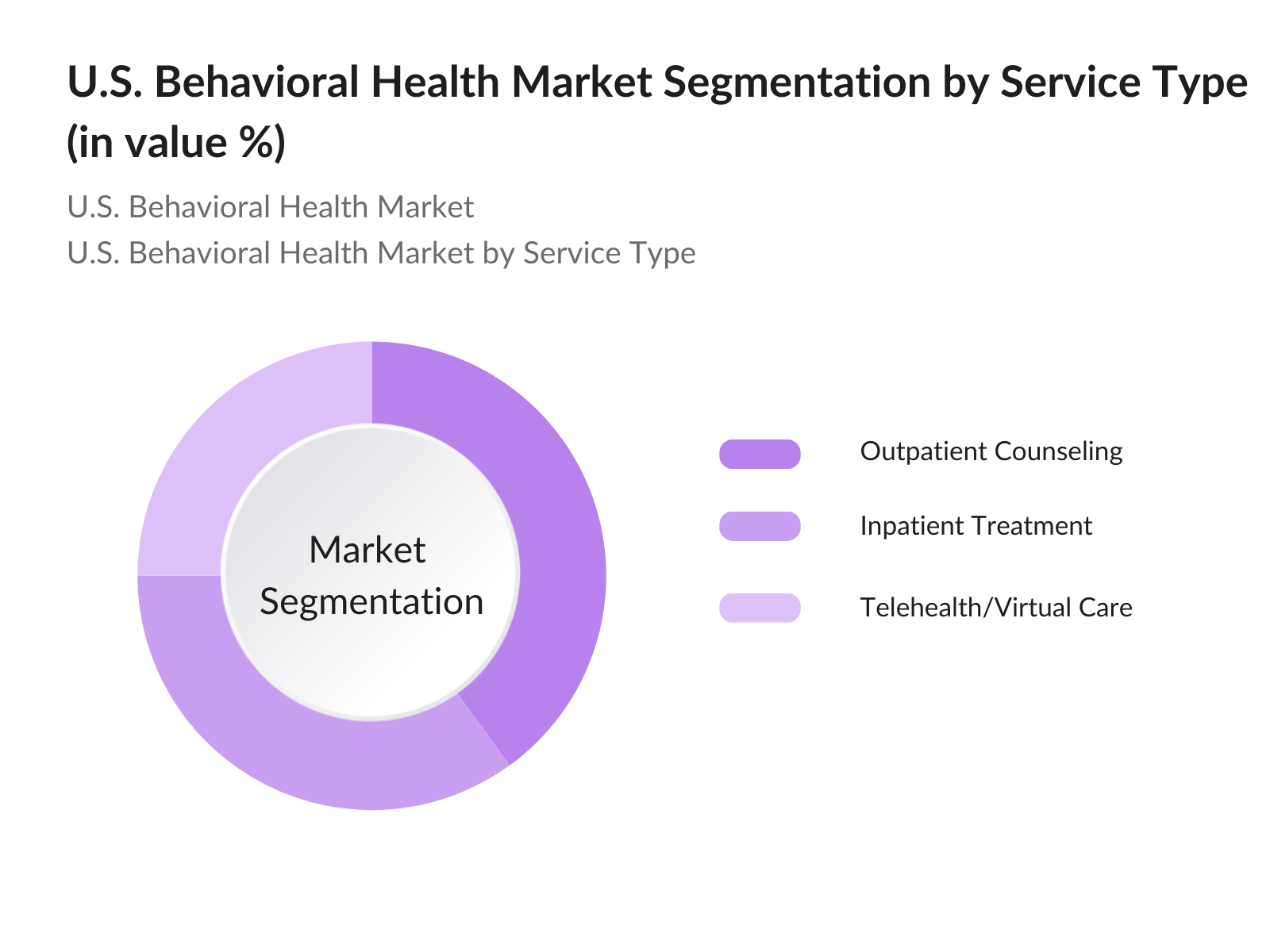
- By Service Type: The U.S. behavioral health market is segmented by service type into outpatient counseling, inpatient treatment, and telehealth/virtual care. Outpatient counseling services have the largest share due to the flexibility and affordability they offer patients, as well as their widespread availability. In recent years, the demand for telehealth services has surged, especially following the COVID-19 pandemic, as patients sought remote care options. Telehealth services continue to grow but outpatient counseling remains the most accessible form of care for mental health and substance use disorders.
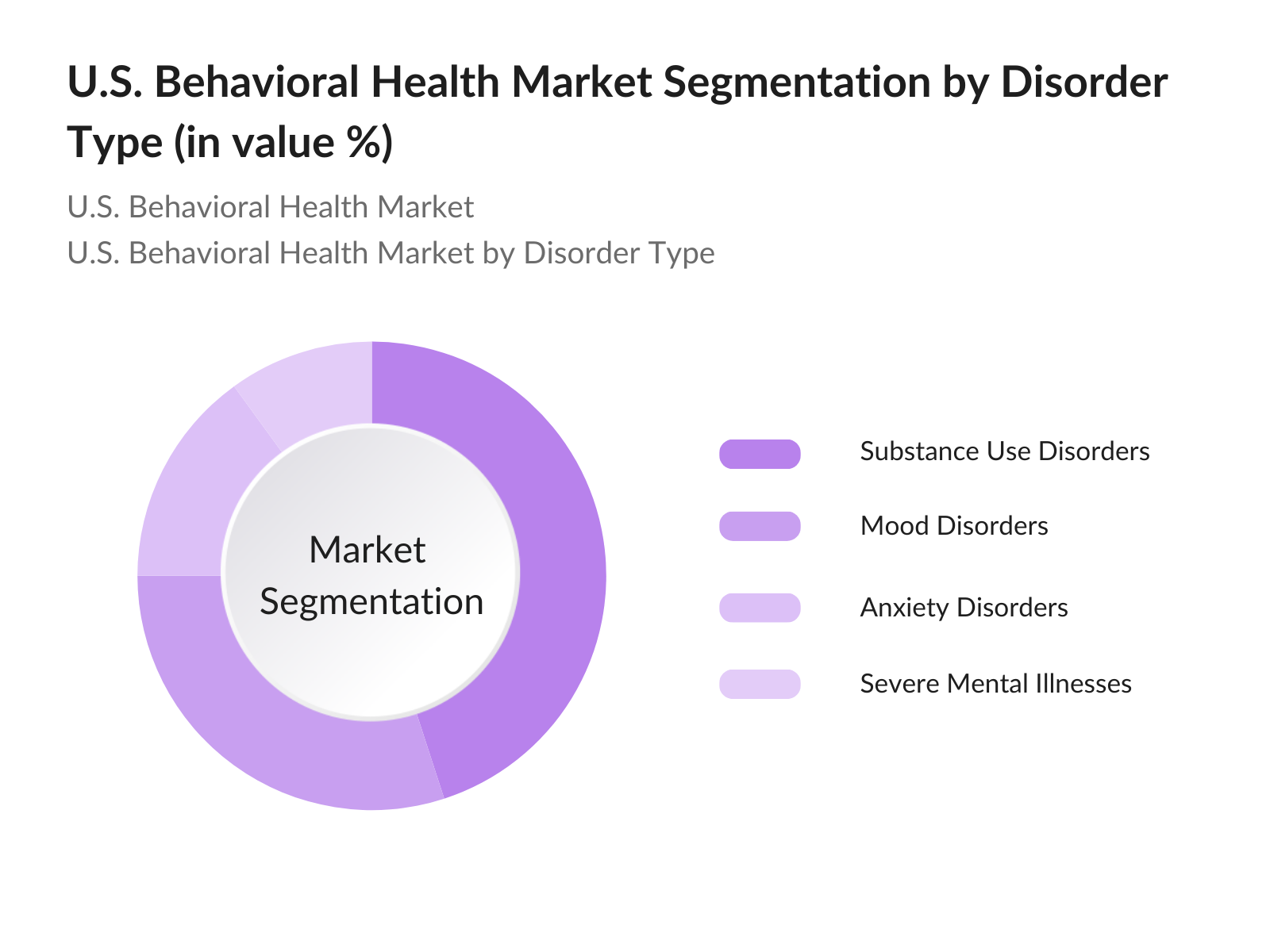
- By Disorder Type: The market is segmented by disorder type into substance use disorders, mood disorders (depression, bipolar disorder), anxiety disorders (PTSD, OCD), and severe mental illnesses such as schizophrenia. Substance use disorders dominate due to the opioid epidemic and the increasing number of people seeking treatment for alcohol and drug-related problems. Government efforts to address these issues through legislation and expanded treatment access are key drivers for the dominance of this segment.
U.S. Behavioral Health Market Competitive Landscape
The U.S. Behavioral Health market is characterized by a mix of large healthcare companies, insurers, and specialized behavioral health service providers. The market is competitive, with major players offering a wide range of services, from inpatient care to outpatient counseling and virtual care. The following table lists the top five players in the U.S. behavioral health market, showcasing their key attributes.
|
Company Name |
Established Year |
Headquarters |
No. of Facilities |
Service Range |
Annual Revenue (USD Bn) |
Reimbursement Model |
Key Partnerships |
Telehealth Offering |
Technology Integration |
|
Universal Health Services (UHS) |
1979 |
King of Prussia, PA |
400+ |
- |
- |
- |
- |
- |
- |
|
Acadia Healthcare |
2005 |
Franklin, TN |
230+ |
- |
- |
- |
- |
- |
- |
|
Magellan Health |
1969 |
Phoenix, AZ |
80+ |
- |
- |
- |
- |
- |
- |
|
Anthem Inc. |
1944 |
Indianapolis, IN |
N/A |
- |
- |
- |
- |
- |
- |
|
Beacon Health Options |
1983 |
Boston, MA |
100+ |
- |
- |
- |
- |
- |
- |
U.S. Behavioral Health Market Analysis
Market Growth Drivers
- Expansion of Telehealth Services: Telehealth services for behavioral health have seen a sharp increase in usage, driven by the need for accessible care. In 2022, the U.S. saw a rise in telehealth utilization, with behavioral health services becoming a crucial part of healthcare delivery. In 2024, the Department of Health and Human Services (HHS) allocated additional funding of $245 million to support the expansion of telehealth in underserved communities. Telehealth visits offer a cost-effective and accessible solution for behavioral health patients, especially those in rural areas, contributing to wider healthcare access.
- Government Initiatives and Funding (Medicaid, Mental Health Parity Act): Government funding plays a pivotal role in the expansion of behavioral health services. In 2023, Medicaid expenditures on mental health services reached $65 billion, reflecting a significant portion of the overall healthcare budget. The Mental Health Parity and Addiction Equity Act (MHPAEA) has enforced regulations to ensure mental health services receive equal insurance coverage compared to physical health. This act has been vital in reducing out-of-pocket expenses for mental health patients. Federal funding also supports community mental health centers, further broadening the accessibility of these services.
- Increasing Awareness of Mental Health: The increasing awareness of mental health issues across the U.S. has spurred the demand for behavioral health services. In 2023, the U.S. government allocated $3.6 billion in mental health funding under the Substance Abuse and Mental Health Services Administration (SAMHSA). This funding addresses the increasing cases of anxiety, depression, and substance use disorders. SAMHSA reports that approximately 21 million people aged 12 or older needed mental health services in 2023, reflecting the growing need for mental health resources.
Market Challenges:
- Shortage of Behavioral Health Providers: The shortage of licensed behavioral health providers remains a significant challenge in the U.S. healthcare system. In 2023, the Health Resources and Services Administration (HRSA) reported that more than 120 million Americans live in areas designated as mental health professional shortage areas. This shortage has led to longer wait times and reduced access to care, particularly in rural regions. The U.S. currently faces a gap of approximately 6,500 full-time behavioral health professionals to meet the population's needs. Initiatives to expand the workforce include federal loan forgiveness programs for mental health practitioners.
- High Treatment Costs: Behavioral health treatment costs are a considerable barrier for many Americans. In 2022, the average cost for mental health outpatient services ranged from $100 to $200 per session, depending on the provider and location. For those without insurance, this makes ongoing treatment difficult to afford. Although federal programs like Medicaid help reduce costs for low-income individuals, many adults with mental health conditions report delaying or avoiding treatment due to the cost. The Mental Health Parity and Addiction Equity Act has attempted to address these disparities, but high costs remain a significant deterrent.
U.S. Behavioral Health Market Future Outlook
The U.S. behavioral health market is expected to experience significant growth in the coming years. Key factors contributing to this growth include the expansion of telehealth services, ongoing government support, and the increasing integration of behavioral health services within primary care settings. Advances in technology, such as AI-driven behavioral health tools and mobile applications, will continue to drive innovation and improve patient outcomes. As societal stigma around mental health decreases, demand for behavioral health services is anticipated to grow steadily.
Market Opportunities:
- Integration of Digital Tools in Behavioral Health Services: Digital tools, such as mobile health applications and online counseling platforms, offer significant opportunities to improve behavioral health services. In 2023, the U.S. Department of Health and Human Services reported a surge in the use of mental health apps, with over 7 million users across platforms like BetterHelp and Talkspace. Digital interventions provide flexible, cost-effective options for patients who cannot access traditional therapy. Furthermore, AI-driven mental health tools are gaining traction in early diagnosis and personalized care, offering real-time support for individuals facing mental health challenges.
- Public-Private Partnerships: Public-private partnerships (PPPs) present opportunities to enhance the U.S. behavioral health infrastructure. In 2023, the Biden administration announced $500 million in public-private partnerships to address mental health needs, including collaborations with technology firms to develop telehealth platforms and digital interventions. PPPs enable the pooling of resources, expertise, and innovative solutions to expand mental health services to underserved populations. This collaboration model is expected to increase the availability of behavioral health services, especially in regions with limited access to mental health professionals.
Scope of the Report
|
By Service Type |
Outpatient Counseling Inpatient Treatment Telehealth/Virtual Care |
|
By Patient Type |
Adults Adolescents Children |
|
By Disorder Type |
Substance Use Disorders Mood Disorders (Depression, Bipolar) Anxiety Disorders (PTSD, OCD) Severe Mental Illnesses |
|
By End-User |
Hospitals Clinics and Behavioral Health Centers Residential Care Facilities |
|
By Region |
North-East Midwest West Coast Southern States |
Products
Key Target Audience
Behavioral Health Providers
Telehealth Companies
Government Agencies (SAMHSA, Medicaid, Medicare)
Health Insurance Companies
Hospitals and Clinics
Substance Abuse Treatment Centers
Investments and Venture Capitalist Firms
Technology Companies (Focused on AI in Healthcare)
Companies
Players Mentioned in the market
Universal Health Services (UHS)
Acadia Healthcare
Magellan Health
Anthem Inc.
Beacon Health Options
Kaiser Permanente
Cigna
UnitedHealth Group
CVS Health/Aetna
New Directions Behavioral Health
Talkspace
Mindful Care
Hopebridge
The Emily Program
Molina Healthcare
Table of Contents
1. U.S. Behavioral Health Market Overview
1.1. Definition and Scope
1.2. Market Taxonomy
1.3. Market Growth Rate
1.4. Market Segmentation Overview
2. U.S. Behavioral Health Market Size (In USD Bn)
2.1. Historical Market Size
2.2. Year-On-Year Growth Analysis
2.3. Key Market Developments and Milestones
3. U.S. Behavioral Health Market Analysis
3.1. Growth Drivers
3.1.2. Expansion of Telehealth Services
3.1.3. Increasing Awareness of Mental Health
3.1.4. Government Initiatives and Funding (Medicaid, Mental Health Parity Act)
3.2. Market Challenges
3.2.1. Shortage of Behavioral Health Providers
3.2.2. High Treatment Costs
3.2.3. Fragmented Reimbursement Systems
3.3. Opportunities
3.3.1. Integration of Digital Tools in Behavioral Health Services
3.3.2. Public-Private Partnerships
3.3.3. Value-Based Care Models in Behavioral Health
3.4. Trends
3.4.1. Growing Focus on Trauma-Informed Care
3.4.2. Expansion of Virtual Behavioral Health Services
3.4.3. Increasing Use of Behavioral Health Apps and Tools
3.5. Government Regulation
3.5. 1. Affordable Care Act (ACA) Impact on Mental Health Coverage
3.5. 2. Mental Health Parity and Addiction Equity Act (MHPAEA)
3.5. 3. Substance Abuse and Mental Health Services Administration (SAMHSA) Regulations
3.6. SWOT Analysis
3.7. Stake Ecosystem
3.8. Porters Five Forces
3.9. Competition Ecosystem
4. U.S. Behavioral Health Market Segmentation
4.1. By Service Type (In Value %)
4.1. 2. Outpatient Counseling
4.1. 3. Inpatient Treatment
4.1.4. Telehealth/Virtual Care
4.2. By Patient Type (In Value %)
4.2.1. Adults
4.2.2. Adolescents
4.2.3. Children
4.3. By Disorder Type (In Value %)
4.3.1. Substance Use Disorders
4.3.2. Mood Disorders (Depression, Bipolar)
4.3.3. Anxiety Disorders (PTSD, OCD)
4.3.4. Severe Mental Illnesses (Schizophrenia, Personality Disorders)
5. Behavioral Health Market Competitive Analysis
5.1 Detailed Profiles of Major Companies
5.1.1. Universal Health Services
5.1.2. Acadia Healthcare
5.1.3. Magellan Health
5.1.4. Anthem Inc.
5.1.5. Centene Corporation
5.1.6. Beacon Health Options
5.1.7. Kaiser Permanente
5.1.8. Cigna
5.1.9. UnitedHealth Group
5.1.10. CVS Health/Aetna
5.1.11. New Directions Behavioral Health
5.1.12. Talkspace
5.1.13. Mindful Care
5.1.14. Hopebridge
5.1.15. The Emily Program
5.2 Cross Comparison Parameters (No. of Facilities, Service Offerings, Revenue, Reimbursement Model, Treatment Specialization, Partnerships, Technology Integration, M&A Activities)
5.3 Market Share Analysis
5.4 Strategic Initiatives
5.5 Mergers and Acquisitions
5.6 Investment Analysis
5.7 Venture Capital Funding
5.8 Government Grants
5.9 Private Equity Investments
6. U.S. Behavioral Health Market Regulatory Framework
6.1. Licensing and Accreditation Standards
6.2. Compliance with HIPAA (Health Insurance Portability and Accountability Act)
6.3. Reimbursement Policies (Medicaid, Medicare)
6.4. Certification Processes
7. U.S. Behavioral Health Future Market Size (In USD Bn)
7.1. Future Market Size Projections
7.2. Key Factors Driving Future Market Growth
8. U.S. Behavioral Health Future Market Segmentation
8.1. By Service Type (In Value %)
8.2. By Patient Type (In Value %)
8.3. By Disorder Type (In Value %)
8.4. By End-User (In Value %)
8.5. By Region (In Value %)
9. U.S. Behavioral Health Market Analysts Recommendations
9.1. TAM/SAM/SOM Analysis
9.2. Customer Cohort Analysis
9.3. Marketing Initiatives
9.4. White Space Opportunity Analysis
Research Methodology
Step 1: Identification of Key Variables
The initial phase involves constructing an ecosystem map encompassing all major stakeholders within the U.S. Behavioral Health Market. This step is underpinned by extensive desk research, utilizing a combination of secondary and proprietary databases to gather comprehensive industry-level information. The primary objective is to identify and define the critical variables that influence market dynamics.
Step 2: Market Analysis and Construction
In this phase, we compile and analyze historical data pertaining to the U.S. Behavioral Health Market. This includes assessing market penetration, service provision, and revenue generation trends. An evaluation of service quality statistics will ensure the reliability and accuracy of revenue estimates.
Step 3: Hypothesis Validation and Expert Consultation
Market hypotheses will be developed and validated through interviews with industry experts, representing a wide range of behavioral health companies. These consultations will provide valuable operational and financial insights that refine the market data and projections.
Step 4: Research Synthesis and Final Output
The final phase involves engaging with multiple healthcare providers to acquire detailed insights into service segments, treatment trends, and consumer behavior. This interaction will serve to verify and complement the statistics derived from the bottom-up approach, ensuring a comprehensive and validated analysis of the U.S. Behavioral Health market.
Frequently Asked Questions
01. How big is the U.S. Behavioral Health Market?
The U.S. behavioral health market is valued at approximately USD 83.78 billion, driven by increased awareness of mental health issues, government support, and the rise of telehealth services.
02. What are the challenges in the U.S. Behavioral Health Market?
The U.S. behavioral health market faces challenges such as the shortage of healthcare providers, high treatment costs, and fragmented reimbursement systems, all of which hinder the overall market growth.
03. Who are the major players in the U.S. Behavioral Health Market?
Key players include Universal Health Services (UHS), Acadia Healthcare, Magellan Health, Anthem Inc., and Beacon Health Options. These companies have strong market positions due to their comprehensive service offerings and national reach.
04. What are the growth drivers of the U.S. Behavioral Health Market?
Growth is driven by factors such as increased telehealth adoption, integration of behavioral health into primary care settings, and growing public awareness of mental health issues.
Why Buy From Us?

What makes us stand out is that our consultants follows Robust, Refine and Result (RRR) methodology. i.e. Robust for clear definitions, approaches and sanity checking, Refine for differentiating respondents facts and opinions and Result for presenting data with story

We have set a benchmark in the industry by offering our clients with syndicated and customized market research reports featuring coverage of entire market as well as meticulous research and analyst insights.

While we don't replace traditional research, we flip the method upside down. Our dual approach of Top Bottom & Bottom Top ensures quality deliverable by not just verifying company fundamentals but also looking at the sector and macroeconomic factors.

With one step in the future, our research team constantly tries to show you the bigger picture. We help with some of the tough questions you may encounter along the way: How is the industry positioned? Best marketing channel? KPI's of competitors? By aligning every element, we help maximize success.

Our report gives you instant access to the answers and sources that other companies might choose to hide. We elaborate each steps of research methodology we have used and showcase you the sample size to earn your trust.

If you need any support, we are here! We pride ourselves on universe strength, data quality, and quick, friendly, and professional service.