About the Report
Base Year 2024Global Technology Solutions in the Healthcare Payer Market Overview
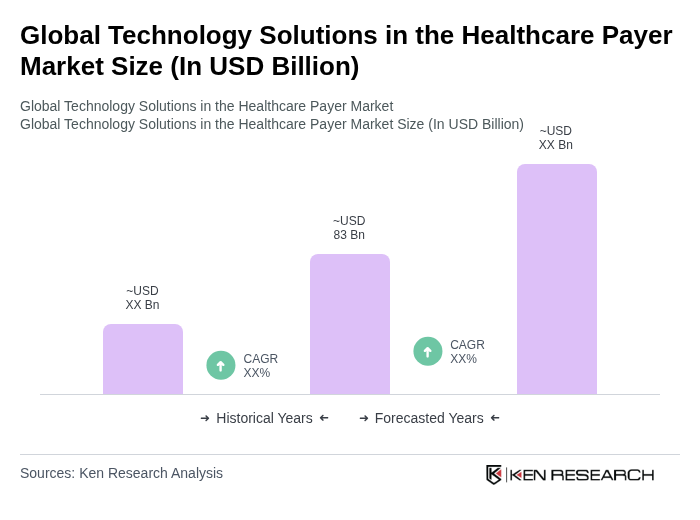
- The Global Technology Solutions in the Healthcare Payer Market is valued at USD 83 billion, based on a five-year historical analysis. This growth is primarily driven by the increasing demand for efficient claims processing, enhanced patient management systems, and the need for robust fraud detection mechanisms. The rising healthcare costs, digital transformation, and the shift towards value-based care models have further accelerated the adoption of technology solutions in this sector. Artificial intelligence, robotic process automation, and advanced analytics are increasingly being integrated to streamline operations, reduce administrative costs, and improve patient outcomes .
- Key players in this market include the United States, Germany, and the United Kingdom. The dominance of these countries is attributed to their advanced healthcare infrastructure, significant investments in health IT, and a high prevalence of private health insurance. Additionally, regulatory frameworks such as the European Health Data Space in the European Union and federal mandates in the United States support innovation and the integration of technology in healthcare services .
- In 2023, the U.S. government implemented the No Surprises Act, which aims to protect patients from unexpected medical bills. This regulation, titled "No Surprises Act, 2021" and issued by the U.S. Department of Health and Human Services, mandates that healthcare providers and insurers must provide clear information about costs and coverage, thereby promoting transparency and accountability in the healthcare payer market. The Act requires compliance with disclosure standards, dispute resolution processes, and cost-sharing protections for patients .
Global Technology Solutions in the Healthcare Payer Market Segmentation
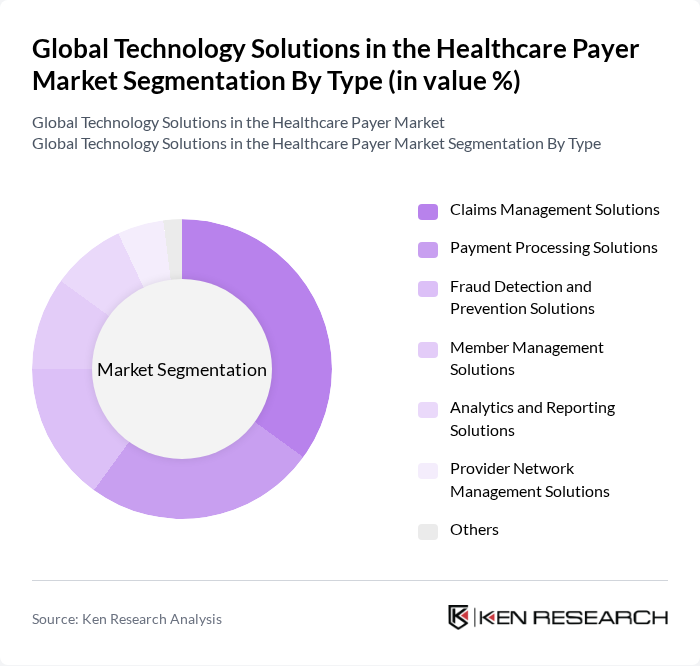
By Type:The technology solutions in the healthcare payer market can be categorized into several types, including Claims Management Solutions, Payment Processing Solutions, Fraud Detection and Prevention Solutions, Member Management Solutions, Analytics and Reporting Solutions, Provider Network Management Solutions, and Others. Among these, Claims Management Solutions are currently leading the market due to the increasing complexity of healthcare claims and the need for efficient processing systems. The demand for streamlined claims management is driven by the growing number of insurance claims, regulatory requirements for timely reimbursement, and the adoption of automation and AI to reduce manual errors and accelerate payment cycles .
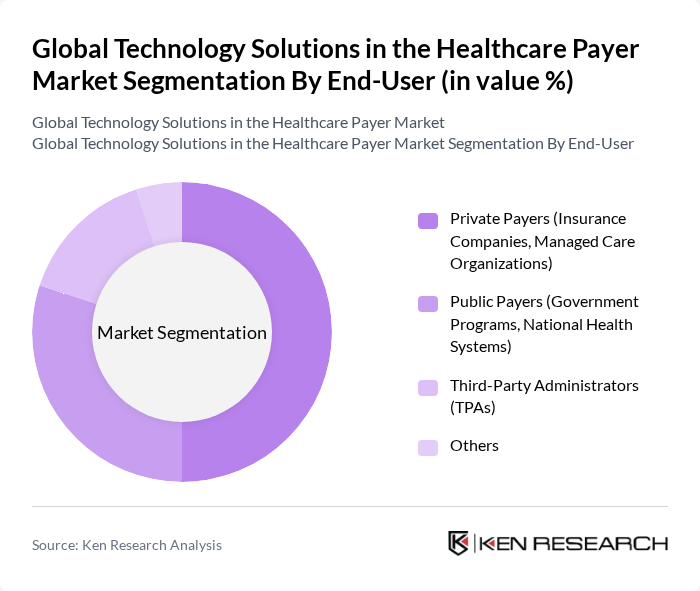
By End-User:The end-users of technology solutions in the healthcare payer market include Private Payers (Insurance Companies, Managed Care Organizations), Public Payers (Government Programs, National Health Systems), Third-Party Administrators (TPAs), and Others. Private Payers dominate this segment as they are increasingly adopting technology solutions to enhance operational efficiency, improve customer service, and comply with evolving regulatory standards. The competitive landscape among private payers drives innovation and the adoption of advanced technologies such as cloud computing, AI, and digital member engagement platforms to meet the evolving needs of consumers .
Global Technology Solutions in the Healthcare Payer Market Competitive Landscape
The Global Technology Solutions in the Healthcare Payer Market is characterized by a dynamic mix of regional and international players. Leading participants such as Optum (UnitedHealth Group), Cognizant Technology Solutions, Change Healthcare (part of Optum/UnitedHealth Group), Tata Consultancy Services (TCS), Accenture, IBM (Watson Health/IBM Health), Oracle Health (formerly Cerner), Infosys, Conduent, EXL Service, Wipro, NTT DATA, Cognizant TriZetto, McKesson Corporation, and HealthEdge Software contribute to innovation, geographic expansion, and service delivery in this space.
Global Technology Solutions in the Healthcare Payer Market Industry Analysis
Growth Drivers
- Increasing Demand for Digital Health Solutions:The global digital health market is projected to reach $508.8 billion in future, driven by a surge in telehealth services and mobile health applications. In future, the telehealth market alone was valued at $57.5 billion, reflecting a 26% increase from the previous year. This growth is fueled by the need for remote patient monitoring and virtual consultations, particularly in regions with limited access to healthcare facilities, enhancing overall patient care and accessibility.
- Rising Healthcare Costs and Need for Efficiency:Healthcare spending in the U.S. is expected to exceed $4.6 trillion in future, prompting payers to seek cost-effective solutions. The implementation of technology solutions can reduce administrative costs by up to $1.7 billion annually for large healthcare organizations. This financial pressure drives the adoption of automated systems and data analytics, which streamline operations and improve resource allocation, ultimately enhancing patient outcomes and operational efficiency.
- Regulatory Support for Technology Adoption:In future, the U.S. government is expected to allocate $1.5 billion to support the integration of technology in healthcare. Initiatives like the CMS's push for value-based care are encouraging payers to adopt innovative solutions. Regulatory frameworks are evolving to facilitate the use of digital health technologies, ensuring compliance while promoting the adoption of electronic health records and telemedicine, which are essential for modern healthcare delivery.
Market Challenges
- Data Security and Privacy Concerns:With healthcare data breaches affecting over 45 million individuals in future, data security remains a significant challenge. The average cost of a data breach in healthcare is approximately $10.1 million, highlighting the financial risks associated with inadequate security measures. As technology adoption increases, so does the vulnerability to cyberattacks, necessitating robust security protocols to protect sensitive patient information and maintain trust in digital health solutions.
- Integration with Legacy Systems:Many healthcare organizations still rely on outdated legacy systems, which complicate the integration of new technologies. Approximately 70% of healthcare providers report challenges in interoperability, leading to inefficiencies and increased operational costs. The inability to seamlessly connect new solutions with existing infrastructure can hinder the adoption of innovative technologies, ultimately affecting patient care and organizational performance in the healthcare payer market.
Global Technology Solutions in the Healthcare Payer Market Future Outlook
The future of technology solutions in the healthcare payer market is poised for significant transformation, driven by advancements in artificial intelligence and machine learning. As healthcare organizations increasingly prioritize patient engagement and data analytics, the demand for interoperable systems will rise. Additionally, the expansion of telehealth services is expected to enhance access to care, particularly in underserved areas, while regulatory support will continue to facilitate the adoption of innovative technologies, ensuring a more efficient and patient-centered healthcare system.
Market Opportunities
- Expansion of Telehealth Services:The telehealth market is projected to grow to $66.5 billion in future, driven by increased consumer acceptance and regulatory support. This presents a significant opportunity for healthcare payers to invest in telehealth platforms, enhancing patient access and satisfaction while reducing costs associated with in-person visits.
- Growth in Artificial Intelligence Applications:The AI healthcare market is expected to reach $45.2 billion in future, offering opportunities for payers to leverage AI for predictive analytics and personalized care. By integrating AI solutions, healthcare organizations can improve decision-making processes, optimize resource allocation, and enhance patient outcomes, ultimately driving efficiency and cost savings.
Scope of the Report
| Segment | Sub-Segments |
|---|---|
| By Type | Claims Management Solutions Payment Processing Solutions Fraud Detection and Prevention Solutions Member Management Solutions Analytics and Reporting Solutions Provider Network Management Solutions Others |
| By End-User | Private Payers (Insurance Companies, Managed Care Organizations) Public Payers (Government Programs, National Health Systems) Third-Party Administrators (TPAs) Others |
| By Service Model | Business Process Outsourcing (BPO) Information Technology Outsourcing (ITO) Knowledge Process Outsourcing (KPO) Software as a Service (SaaS) Platform as a Service (PaaS) Infrastructure as a Service (IaaS) Others |
| By Deployment Mode | On-Premises Cloud-Based Hybrid Others |
| By Functionality | Billing and Coding Patient Management Reporting and Analytics Provider Data Management Fraud Detection Others |
| By Region | North America Europe Asia-Pacific Latin America Middle East & Africa |
| By Policy Support | Government Subsidies Tax Incentives Regulatory Support Programs Others |
Key Target Audience
Investors and Venture Capitalist Firms
Government and Regulatory Bodies (e.g., Centers for Medicare & Medicaid Services, Food and Drug Administration)
Healthcare Insurance Providers
Healthcare Technology Solution Developers
Pharmaceutical Benefit Managers
Healthcare Data Analytics Firms
Health Information Exchange Organizations
Healthcare Compliance and Risk Management Firms
Players Mentioned in the Report:
Optum (UnitedHealth Group)
Cognizant Technology Solutions
Change Healthcare (part of Optum/UnitedHealth Group)
Tata Consultancy Services (TCS)
Accenture
IBM (Watson Health/IBM Health)
Oracle Health (formerly Cerner)
Infosys
Conduent
EXL Service
Wipro
NTT DATA
Cognizant TriZetto
McKesson Corporation
HealthEdge Software
Table of Contents
Market Assessment Phase
1. Executive Summary and Approach
2. Global Technology Solutions in the Healthcare Payer Market Overview
2.1 Key Insights and Strategic Recommendations
2.2 Global Technology Solutions in the Healthcare Payer Market Overview
2.3 Definition and Scope
2.4 Evolution of Market Ecosystem
2.5 Timeline of Key Regulatory Milestones
2.6 Value Chain & Stakeholder Mapping
2.7 Business Cycle Analysis
2.8 Policy & Incentive Landscape
3. Global Technology Solutions in the Healthcare Payer Market Analysis
3.1 Growth Drivers
3.1.1 Increasing Demand for Digital Health Solutions
3.1.2 Rising Healthcare Costs and Need for Efficiency
3.1.3 Regulatory Support for Technology Adoption
3.1.4 Shift Towards Value-Based Care Models
3.2 Market Challenges
3.2.1 Data Security and Privacy Concerns
3.2.2 Integration with Legacy Systems
3.2.3 High Initial Investment Costs
3.2.4 Resistance to Change from Stakeholders
3.3 Market Opportunities
3.3.1 Expansion of Telehealth Services
3.3.2 Growth in Artificial Intelligence Applications
3.3.3 Increasing Focus on Patient Engagement Tools
3.3.4 Development of Interoperable Systems
3.4 Market Trends
3.4.1 Rise of Cloud-Based Solutions
3.4.2 Adoption of Blockchain Technology
3.4.3 Emphasis on Data Analytics and Insights
3.4.4 Growth of Mobile Health Applications
3.5 Government Regulation
3.5.1 HIPAA Compliance Requirements
3.5.2 FDA Regulations on Digital Health Technologies
3.5.3 CMS Initiatives for Value-Based Care
3.5.4 Data Protection Laws and Guidelines
4. SWOT Analysis
5. Stakeholder Analysis
6. Porter's Five Forces Analysis
7. Global Technology Solutions in the Healthcare Payer Market Market Size, 2019-2024
7.1 By Value
7.2 By Volume
7.3 By Average Selling Price
8. Global Technology Solutions in the Healthcare Payer Market Segmentation
8.1 By Type
8.1.1 Claims Management Solutions
8.1.2 Payment Processing Solutions
8.1.3 Fraud Detection and Prevention Solutions
8.1.4 Member Management Solutions
8.1.5 Analytics and Reporting Solutions
8.1.6 Provider Network Management Solutions
8.1.7 Others
8.2 By End-User
8.2.1 Private Payers (Insurance Companies, Managed Care Organizations)
8.2.2 Public Payers (Government Programs, National Health Systems)
8.2.3 Third-Party Administrators (TPAs)
8.2.4 Others
8.3 By Service Model
8.3.1 Business Process Outsourcing (BPO)
8.3.2 Information Technology Outsourcing (ITO)
8.3.3 Knowledge Process Outsourcing (KPO)
8.3.4 Software as a Service (SaaS)
8.3.5 Platform as a Service (PaaS)
8.3.6 Infrastructure as a Service (IaaS)
8.3.7 Others
8.4 By Deployment Mode
8.4.1 On-Premises
8.4.2 Cloud-Based
8.4.3 Hybrid
8.4.4 Others
8.5 By Functionality
8.5.1 Billing and Coding
8.5.2 Patient Management
8.5.3 Reporting and Analytics
8.5.4 Provider Data Management
8.5.5 Fraud Detection
8.5.6 Others
8.6 By Region
8.6.1 North America
8.6.2 Europe
8.6.3 Asia-Pacific
8.6.4 Latin America
8.6.5 Middle East & Africa
8.7 By Policy Support
8.7.1 Government Subsidies
8.7.2 Tax Incentives
8.7.3 Regulatory Support Programs
8.7.4 Others
9. Global Technology Solutions in the Healthcare Payer Market Competitive Analysis
9.1 Market Share of Key Players
9.2 Cross Comparison of Key Players
9.2.1 Company Name
9.2.2 Group Size (Large, Medium, or Small as per industry convention)
9.2.3 Revenue Growth Rate
9.2.4 Market Share in Healthcare Payer Technology Solutions
9.2.5 Number of Payer Clients / Covered Lives
9.2.6 Customer Acquisition Cost
9.2.7 Customer Retention Rate
9.2.8 Market Penetration Rate (by geography or segment)
9.2.9 Pricing Strategy (Subscription, Transaction-based, etc.)
9.2.10 Average Deal Size
9.2.11 Return on Investment (ROI) for Clients
9.2.12 Net Promoter Score (NPS)
9.2.13 R&D Spend as % of Revenue
9.2.14 Technology Innovation Index (e.g., patents, AI/ML capabilities)
9.3 SWOT Analysis of Top Players
9.4 Pricing Analysis
9.5 Detailed Profile of Major Companies
9.5.1 Optum (UnitedHealth Group)
9.5.2 Cognizant Technology Solutions
9.5.3 Change Healthcare (part of Optum/UnitedHealth Group)
9.5.4 Tata Consultancy Services (TCS)
9.5.5 Accenture
9.5.6 IBM (Watson Health/IBM Health)
9.5.7 Oracle Health (formerly Cerner)
9.5.8 Infosys
9.5.9 Conduent
9.5.10 EXL Service
9.5.11 Wipro
9.5.12 NTT DATA
9.5.13 Cognizant TriZetto
9.5.14 McKesson Corporation
9.5.15 HealthEdge Software
10. Global Technology Solutions in the Healthcare Payer Market End-User Analysis
10.1 Procurement Behavior of Key Ministries
10.1.1 Budget Allocation Trends
10.1.2 Decision-Making Processes
10.1.3 Vendor Selection Criteria
10.1.4 Others
10.2 Corporate Spend on Infrastructure & Energy
10.2.1 Investment Priorities
10.2.2 Spending Patterns
10.2.3 Cost Management Strategies
10.2.4 Others
10.3 Pain Point Analysis by End-User Category
10.3.1 Common Challenges Faced
10.3.2 Technology Gaps
10.3.3 Service Delivery Issues
10.3.4 Others
10.4 User Readiness for Adoption
10.4.1 Training and Support Needs
10.4.2 Technology Familiarity
10.4.3 Change Management Readiness
10.4.4 Others
10.5 Post-Deployment ROI and Use Case Expansion
10.5.1 Performance Metrics
10.5.2 User Feedback and Satisfaction
10.5.3 Scalability of Solutions
10.5.4 Others
11. Global Technology Solutions in the Healthcare Payer Market Future Size, 2025-2030
11.1 By Value
11.2 By Volume
11.3 By Average Selling Price
Go-To-Market Strategy Phase
1. Whitespace Analysis + Business Model Canvas
1.1 Market Gaps Identification
1.2 Business Model Framework
2. Marketing and Positioning Recommendations
2.1 Branding Strategies
2.2 Product USPs
3. Distribution Plan
3.1 Urban Retail vs Rural NGO Tie-Ups
4. Channel & Pricing Gaps
4.1 Underserved Routes
4.2 Pricing Bands
5. Unmet Demand & Latent Needs
5.1 Category Gaps
5.2 Consumer Segments
6. Customer Relationship
6.1 Loyalty Programs
6.2 After-Sales Service
7. Value Proposition
7.1 Sustainability
7.2 Integrated Supply Chains
8. Key Activities
8.1 Regulatory Compliance
8.2 Branding
8.3 Distribution Setup
9. Entry Strategy Evaluation
9.1 Domestic Market Entry Strategy
9.1.1 Product Mix
9.1.2 Pricing Band
9.1.3 Packaging
9.2 Export Entry Strategy
9.2.1 Target Countries
9.2.2 Compliance Roadmap
10. Entry Mode Assessment
10.1 Joint Ventures
10.2 Greenfield Investments
10.3 Mergers & Acquisitions
10.4 Distributor Model
11. Capital and Timeline Estimation
11.1 Capital Requirements
11.2 Timelines
12. Control vs Risk Trade-Off
12.1 Ownership vs Partnerships
13. Profitability Outlook
13.1 Breakeven Analysis
13.2 Long-Term Sustainability
14. Potential Partner List
14.1 Distributors
14.2 Joint Ventures
14.3 Acquisition Targets
15. Execution Roadmap
15.1 Phased Plan for Market Entry
15.1.1 Market Setup
15.1.2 Market Entry
15.1.3 Growth Acceleration
15.1.4 Scale & Stabilize
15.2 Key Activities and Milestones
15.2.1 Milestone Planning
15.2.2 Activity Tracking
Research Methodology
Phase 1: Approach1
Desk Research
- Analysis of industry reports from healthcare technology associations and market research firms
- Review of published white papers and case studies on technology solutions in healthcare payers
- Examination of regulatory frameworks and compliance guidelines from healthcare authorities
Primary Research
- Interviews with executives from healthcare payer organizations to understand technology adoption trends
- Surveys targeting IT managers and technology leads within healthcare payers to gather insights on current solutions
- Focus groups with healthcare professionals to assess the impact of technology on payer operations
Validation & Triangulation
- Cross-validation of findings through multiple data sources, including market reports and expert opinions
- Triangulation of qualitative insights from interviews with quantitative data from surveys
- Sanity checks conducted through expert panel reviews to ensure data accuracy and relevance
Phase 2: Market Size Estimation1
Top-down Assessment
- Estimation of the total addressable market (TAM) for technology solutions in healthcare payers based on industry spending
- Segmentation of the market by technology type, including AI, data analytics, and cloud solutions
- Incorporation of growth rates from healthcare expenditure forecasts and payer technology investments
Bottom-up Modeling
- Collection of firm-level data from leading technology providers serving healthcare payers
- Estimation of market share based on revenue figures and client portfolios of key players
- Volume x pricing analysis for various technology solutions tailored to payer needs
Forecasting & Scenario Analysis
- Multi-factor regression analysis incorporating variables such as regulatory changes and technological advancements
- Scenario modeling based on potential shifts in healthcare policies and payer operational strategies
- Development of baseline, optimistic, and pessimistic forecasts through 2030
Phase 3: CATI Sample Composition1
| Scope Item/Segment | Sample Size | Target Respondent Profiles |
|---|---|---|
| Healthcare Payer Technology Adoption | 100 | IT Directors, Chief Technology Officers |
| Data Analytics Solutions in Payers | 80 | Data Scientists, Analytics Managers |
| AI Implementation in Claims Processing | 60 | Operations Managers, Claims Analysts |
| Cloud Solutions for Healthcare Payers | 50 | Infrastructure Managers, Cloud Architects |
| Regulatory Compliance Technologies | 40 | Compliance Officers, Risk Management Executives |
Frequently Asked Questions
What is the current value of the Global Technology Solutions in the Healthcare Payer Market?
The Global Technology Solutions in the Healthcare Payer Market is valued at approximately USD 83 billion, driven by the demand for efficient claims processing, enhanced patient management systems, and robust fraud detection mechanisms.