About the Report
Base Year 2024Philippines Healthcare Fraud Analytics Market Overview
- The Philippines Healthcare Fraud Analytics Market is valued at USD 15 million, based on a five-year historical analysis. This growth is primarily driven by the increasing prevalence of healthcare fraud, rising healthcare expenditures, adoption of advanced analytics and AI technologies, and regulatory pressures for compliance and transparency. The market is further propelled by the shift to electronic health records, the need for real-time fraud detection, and the integration of cloud-based analytics solutions, which collectively enhance the ability of healthcare providers and insurers to detect and prevent fraudulent activities .
- Metro Manila, Cebu, and Davao remain the dominant regions in the Philippines Healthcare Fraud Analytics Market. Metro Manila leads due to its high concentration of healthcare facilities, insurance companies, and digital health infrastructure, while Cebu and Davao benefit from expanding healthcare networks and increased awareness of fraud detection technologies among local providers .
- The Universal Health Care Act (Republic Act No. 11223), issued by the Philippine Congress in 2019 and implemented by the Department of Health and PhilHealth, mandates the establishment of a comprehensive healthcare fraud detection and prevention system. This regulation requires healthcare providers to adopt analytics solutions for claims monitoring, compliance with health insurance policies, and reporting of suspicious activities, thereby enhancing the integrity and transparency of the national healthcare system .
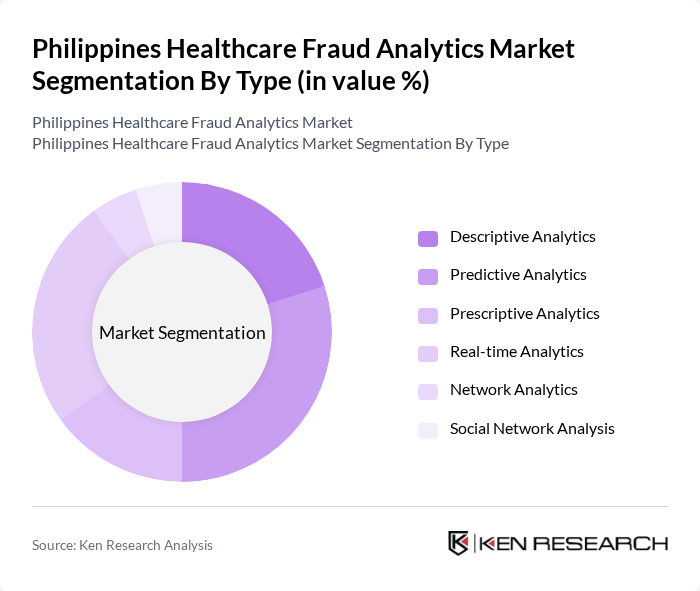
Philippines Healthcare Fraud Analytics Market Segmentation
By Type:The market is segmented into various types of analytics solutions that address different aspects of fraud detection and prevention. The subsegments includeDescriptive Analytics(for identifying historical patterns and trends),Predictive Analytics(for forecasting potential fraud risks using statistical models and machine learning),Prescriptive Analytics(for recommending optimal responses to detected fraud),Real-time Analytics(for immediate detection and intervention),Network Analytics(for uncovering fraud rings and collusion), andSocial Network Analysis(for mapping relationships among entities involved in fraudulent activities). These analytics types are critical for enabling healthcare organizations to proactively identify, predict, and mitigate fraudulent activities .
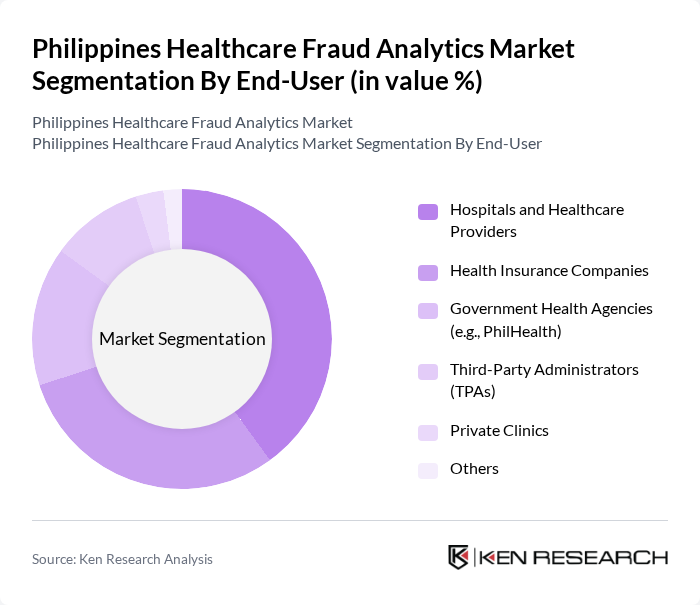
By End-User:The end-user segmentation includesHospitals and Healthcare Providers(leveraging analytics for claims validation and operational efficiency),Health Insurance Companies(using analytics to detect fraudulent claims and reduce financial losses),Government Health Agencies(such as PhilHealth, focusing on compliance and fraud monitoring),Third-Party Administrators (TPAs)(for efficient claims processing and fraud detection),Private Clinics, andOthers. Each segment utilizes fraud analytics to enhance efficiency, minimize fraud-related losses, and improve patient outcomes .
Philippines Healthcare Fraud Analytics Market Competitive Landscape
The Philippines Healthcare Fraud Analytics Market is characterized by a dynamic mix of regional and international players. Leading participants such as SAS Institute Inc., IBM Corporation, Optum, Inc., Oracle Corporation, Cerner Corporation (now Oracle Health), LexisNexis Risk Solutions, Change Healthcare (a part of Optum), Verisk Analytics, Inc., Cotiviti, Inc., Wipro Limited, HealthEdge Software, Inc., NextGen Healthcare, Inc., eClinicalWorks, Philips Healthcare, Medilink Network, Inc., PhilHealth (Philippine Health Insurance Corporation), Ayala Healthcare Holdings, Inc. (AC Health), Zuellig Pharma Philippines contribute to innovation, geographic expansion, and service delivery in this space.
Philippines Healthcare Fraud Analytics Market Industry Analysis
Growth Drivers
- Increasing Incidence of Healthcare Fraud:The Philippines has reported a significant rise in healthcare fraud cases, with estimates indicating losses of approximately PHP 10 billion annually due to fraudulent activities. This alarming trend has prompted healthcare organizations to invest in fraud analytics solutions to mitigate risks. The Philippine Health Insurance Corporation (PhilHealth) has identified over 1,000 cases of fraud in recent years, highlighting the urgent need for effective fraud detection mechanisms to protect public funds and ensure quality healthcare delivery.
- Government Initiatives for Fraud Prevention:The Philippine government has launched several initiatives aimed at combating healthcare fraud, including the establishment of the Anti-Fraud Task Force. This task force is responsible for investigating fraudulent claims and implementing preventive measures. Additionally, the Department of Health allocated PHP 500 million for the development of advanced fraud detection systems, demonstrating a strong commitment to enhancing the integrity of the healthcare system and safeguarding public resources.
- Advancements in Data Analytics Technologies:The rapid evolution of data analytics technologies is transforming the healthcare landscape in the Philippines. In future, the market for healthcare analytics is projected to reach PHP 3 billion, driven by the adoption of advanced tools such as machine learning and artificial intelligence. These technologies enable healthcare providers to analyze vast amounts of data efficiently, identifying patterns and anomalies that indicate potential fraud, thereby enhancing the overall effectiveness of fraud detection efforts.
Market Challenges
- Lack of Standardization in Fraud Detection:One of the significant challenges facing the Philippines healthcare fraud analytics market is the absence of standardized protocols for fraud detection. Currently, various healthcare providers employ different methodologies, leading to inconsistencies in identifying and reporting fraudulent activities. This lack of uniformity complicates the collaboration between stakeholders and hinders the development of comprehensive fraud prevention strategies, ultimately affecting the overall effectiveness of fraud analytics initiatives.
- High Implementation Costs:The financial burden associated with implementing advanced fraud analytics solutions poses a significant challenge for many healthcare organizations in the Philippines. Initial setup costs for sophisticated analytics systems can exceed PHP 2 million, which may deter smaller providers from investing in necessary technologies. Additionally, ongoing maintenance and training expenses further strain budgets, limiting the ability of healthcare providers to adopt comprehensive fraud detection measures effectively.
Philippines Healthcare Fraud Analytics Market Future Outlook
The future of the Philippines healthcare fraud analytics market appears promising, driven by increasing investments in technology and a growing emphasis on regulatory compliance. As healthcare providers recognize the importance of proactive fraud management, the integration of predictive analytics and AI will become more prevalent. Furthermore, collaboration between government agencies and technology firms is expected to enhance the development of innovative solutions, ultimately leading to improved fraud detection capabilities and a more secure healthcare environment.
Market Opportunities
- Growth of Telemedicine Services:The expansion of telemedicine services in the Philippines presents a unique opportunity for fraud analytics. With the increasing number of virtual consultations, the potential for fraudulent claims has also risen. Implementing robust analytics solutions tailored for telehealth can help identify suspicious activities, ensuring that healthcare providers maintain integrity while delivering remote services to patients.
- Integration of AI and Machine Learning:The integration of AI and machine learning technologies into healthcare fraud analytics offers significant potential for enhancing detection capabilities. By leveraging these advanced technologies, healthcare organizations can analyze vast datasets in real-time, identifying patterns indicative of fraud more efficiently. This proactive approach not only reduces financial losses but also fosters trust among patients and stakeholders in the healthcare system.
Scope of the Report
| Segment | Sub-Segments |
|---|---|
| By Type | Descriptive Analytics Predictive Analytics Prescriptive Analytics Real-time Analytics Network Analytics Social Network Analysis |
| By End-User | Hospitals and Healthcare Providers Health Insurance Companies Government Health Agencies (e.g., PhilHealth) Third-Party Administrators (TPAs) Private Clinics Others |
| By Application | Claims Fraud Detection Provider Fraud Detection Payment Integrity Prescription Fraud Detection Identity Theft Detection Others |
| By Deployment Mode | On-Premises Cloud-Based Hybrid |
| By Region | Luzon Visayas Mindanao Metro Manila Others |
| By Pricing Model | Subscription-Based Pay-Per-Use One-Time License Fee |
| By Customer Size | Small Enterprises Medium Enterprises Large Enterprises |
Key Target Audience
Investors and Venture Capitalist Firms
Government and Regulatory Bodies (e.g., Department of Health, National Bureau of Investigation)
Healthcare Providers and Institutions
Insurance Companies and Health Plans
Fraud Detection Technology Developers
Healthcare Compliance Organizations
Law Enforcement Agencies
Healthcare Industry Associations
Players Mentioned in the Report:
SAS Institute Inc.
IBM Corporation
Optum, Inc.
Oracle Corporation
Cerner Corporation (now Oracle Health)
LexisNexis Risk Solutions
Change Healthcare (a part of Optum)
Verisk Analytics, Inc.
Cotiviti, Inc.
Wipro Limited
HealthEdge Software, Inc.
NextGen Healthcare, Inc.
eClinicalWorks
Philips Healthcare
Medilink Network, Inc.
PhilHealth (Philippine Health Insurance Corporation)
Ayala Healthcare Holdings, Inc. (AC Health)
Zuellig Pharma Philippines
Table of Contents
Market Assessment Phase
1. Executive Summary and Approach
2. Philippines Healthcare Fraud Analytics Market Overview
2.1 Key Insights and Strategic Recommendations
2.2 Philippines Healthcare Fraud Analytics Market Overview
2.3 Definition and Scope
2.4 Evolution of Market Ecosystem
2.5 Timeline of Key Regulatory Milestones
2.6 Value Chain & Stakeholder Mapping
2.7 Business Cycle Analysis
2.8 Policy & Incentive Landscape
3. Philippines Healthcare Fraud Analytics Market Analysis
3.1 Growth Drivers
3.1.1 Increasing Incidence of Healthcare Fraud
3.1.2 Government Initiatives for Fraud Prevention
3.1.3 Advancements in Data Analytics Technologies
3.1.4 Rising Awareness Among Healthcare Providers
3.2 Market Challenges
3.2.1 Lack of Standardization in Fraud Detection
3.2.2 High Implementation Costs
3.2.3 Resistance to Change Among Stakeholders
3.2.4 Data Privacy Concerns
3.3 Market Opportunities
3.3.1 Growth of Telemedicine Services
3.3.2 Integration of AI and Machine Learning
3.3.3 Expansion of Health Insurance Coverage
3.3.4 Collaboration with Technology Providers
3.4 Market Trends
3.4.1 Increasing Use of Predictive Analytics
3.4.2 Shift Towards Proactive Fraud Management
3.4.3 Enhanced Regulatory Scrutiny
3.4.4 Adoption of Blockchain for Data Security
3.5 Government Regulation
3.5.1 Implementation of the Universal Health Care Law
3.5.2 Data Privacy Act Compliance
3.5.3 Anti-Fraud Regulations by the Department of Health
3.5.4 Guidelines from the Insurance Commission
4. SWOT Analysis
5. Stakeholder Analysis
6. Porter's Five Forces Analysis
7. Philippines Healthcare Fraud Analytics Market Market Size, 2019-2024
7.1 By Value
7.2 By Volume
7.3 By Average Selling Price
8. Philippines Healthcare Fraud Analytics Market Segmentation
8.1 By Type
8.1.1 Descriptive Analytics
8.1.2 Predictive Analytics
8.1.3 Prescriptive Analytics
8.1.4 Real-time Analytics
8.1.5 Network Analytics
8.1.6 Social Network Analysis
8.2 By End-User
8.2.1 Hospitals and Healthcare Providers
8.2.2 Health Insurance Companies
8.2.3 Government Health Agencies (e.g., PhilHealth)
8.2.4 Third-Party Administrators (TPAs)
8.2.5 Private Clinics
8.2.6 Others
8.3 By Application
8.3.1 Claims Fraud Detection
8.3.2 Provider Fraud Detection
8.3.3 Payment Integrity
8.3.4 Prescription Fraud Detection
8.3.5 Identity Theft Detection
8.3.6 Others
8.4 By Deployment Mode
8.4.1 On-Premises
8.4.2 Cloud-Based
8.4.3 Hybrid
8.5 By Region
8.5.1 Luzon
8.5.2 Visayas
8.5.3 Mindanao
8.5.4 Metro Manila
8.5.5 Others
8.6 By Pricing Model
8.6.1 Subscription-Based
8.6.2 Pay-Per-Use
8.6.3 One-Time License Fee
8.7 By Customer Size
8.7.1 Small Enterprises
8.7.2 Medium Enterprises
8.7.3 Large Enterprises
9. Philippines Healthcare Fraud Analytics Market Competitive Analysis
9.1 Market Share of Key Players
9.2 Cross Comparison of Key Players
9.2.1 Company Name
9.2.2 Group Size (Large, Medium, or Small as per industry convention)
9.2.3 Revenue Growth Rate (Philippines Healthcare Fraud Analytics Segment)
9.2.4 Number of Healthcare Clients in the Philippines
9.2.5 Market Share in Philippines Healthcare Fraud Analytics
9.2.6 Customer Acquisition Cost (CAC)
9.2.7 Customer Retention Rate
9.2.8 Average Implementation Time (in weeks)
9.2.9 Average Deal Size (USD)
9.2.10 Return on Investment (ROI) for Clients
9.2.11 Detection Accuracy Rate (%)
9.2.12 False Positive Rate (%)
9.2.13 Compliance with Local Regulations (e.g., Data Privacy Act)
9.2.14 Local Support Presence
9.2.15 Product Innovation Index
9.3 SWOT Analysis of Top Players
9.4 Pricing Analysis
9.5 Detailed Profile of Major Companies
9.5.1 SAS Institute Inc.
9.5.2 IBM Corporation
9.5.3 Optum, Inc.
9.5.4 Oracle Corporation
9.5.5 Cerner Corporation (now Oracle Health)
9.5.6 LexisNexis Risk Solutions
9.5.7 Change Healthcare (a part of Optum)
9.5.8 Verisk Analytics, Inc.
9.5.9 Cotiviti, Inc.
9.5.10 Wipro Limited
9.5.11 HealthEdge Software, Inc.
9.5.12 NextGen Healthcare, Inc.
9.5.13 eClinicalWorks
9.5.14 Philips Healthcare
9.5.15 Medilink Network, Inc.
9.5.16 PhilHealth (Philippine Health Insurance Corporation)
9.5.17 Ayala Healthcare Holdings, Inc. (AC Health)
9.5.18 Zuellig Pharma Philippines
10. Philippines Healthcare Fraud Analytics Market End-User Analysis
10.1 Procurement Behavior of Key Ministries
10.1.1 Budget Allocation for Fraud Prevention
10.1.2 Decision-Making Processes
10.1.3 Preferred Procurement Channels
10.2 Corporate Spend on Infrastructure & Energy
10.2.1 Investment in Fraud Detection Technologies
10.2.2 Spending on Training and Development
10.2.3 Budget for Compliance and Regulatory Needs
10.3 Pain Point Analysis by End-User Category
10.3.1 Challenges in Data Integration
10.3.2 Difficulty in Real-Time Monitoring
10.3.3 Need for User-Friendly Interfaces
10.4 User Readiness for Adoption
10.4.1 Training Needs Assessment
10.4.2 Technology Adoption Barriers
10.4.3 Stakeholder Engagement Strategies
10.5 Post-Deployment ROI and Use Case Expansion
10.5.1 Measurement of Fraud Reduction
10.5.2 Expansion into New Use Cases
10.5.3 Long-Term Cost Savings Analysis
11. Philippines Healthcare Fraud Analytics Market Future Size, 2025-2030
11.1 By Value
11.2 By Volume
11.3 By Average Selling Price
Go-To-Market Strategy Phase
1. Whitespace Analysis + Business Model Canvas
1.1 Identification of Market Gaps
1.2 Value Proposition Development
1.3 Revenue Streams Analysis
1.4 Key Partnerships
1.5 Cost Structure Evaluation
1.6 Customer Segmentation
1.7 Channels of Distribution
2. Marketing and Positioning Recommendations
2.1 Branding Strategies
2.2 Product USPs
2.3 Target Audience Identification
2.4 Communication Strategies
2.5 Digital Marketing Approaches
3. Distribution Plan
3.1 Urban Retail Strategies
3.2 Rural NGO Tie-Ups
3.3 Online Distribution Channels
3.4 Partnerships with Healthcare Providers
4. Channel & Pricing Gaps
4.1 Underserved Routes
4.2 Pricing Bands Analysis
4.3 Competitor Pricing Strategies
4.4 Customer Willingness to Pay
5. Unmet Demand & Latent Needs
5.1 Category Gaps
5.2 Consumer Segments Analysis
5.3 Emerging Trends in Consumer Behavior
5.4 Future Needs Assessment
6. Customer Relationship
6.1 Loyalty Programs
6.2 After-Sales Service
6.3 Customer Feedback Mechanisms
6.4 Engagement Strategies
7. Value Proposition
7.1 Sustainability Initiatives
7.2 Integrated Supply Chains
7.3 Unique Selling Points
7.4 Customer-Centric Approaches
8. Key Activities
8.1 Regulatory Compliance
8.2 Branding Initiatives
8.3 Distribution Setup
8.4 Training and Development
9. Entry Strategy Evaluation
9.1 Domestic Market Entry Strategy
9.1.1 Product Mix Considerations
9.1.2 Pricing Band Strategies
9.1.3 Packaging Innovations
9.2 Export Entry Strategy
9.2.1 Target Countries Identification
9.2.2 Compliance Roadmap Development
10. Entry Mode Assessment
10.1 Joint Ventures
10.2 Greenfield Investments
10.3 Mergers & Acquisitions
10.4 Distributor Model Evaluation
11. Capital and Timeline Estimation
11.1 Capital Requirements Analysis
11.2 Timelines for Market Entry
12. Control vs Risk Trade-Off
12.1 Ownership vs Partnerships
12.2 Risk Management Strategies
13. Profitability Outlook
13.1 Breakeven Analysis
13.2 Long-Term Sustainability Strategies
14. Potential Partner List
14.1 Distributors
14.2 Joint Ventures
14.3 Acquisition Targets
15. Execution Roadmap
15.1 Phased Plan for Market Entry
15.1.1 Market Setup
15.1.2 Market Entry
15.1.3 Growth Acceleration
15.1.4 Scale & Stabilize
15.2 Key Activities and Milestones
15.2.1 Milestone Planning
15.2.2 Activity Tracking
Research Methodology
Phase 1: Approach1
Desk Research
- Analysis of healthcare expenditure reports from the Philippine Statistics Authority
- Review of published studies on healthcare fraud trends in the Philippines
- Examination of regulatory frameworks and guidelines from the Department of Health
Primary Research
- Interviews with healthcare compliance officers from hospitals and clinics
- Surveys with insurance fraud investigators and auditors
- Focus groups with healthcare professionals discussing fraud detection practices
Validation & Triangulation
- Cross-validation of findings with data from healthcare fraud case studies
- Triangulation of insights from primary interviews and secondary data sources
- Sanity checks through expert panel discussions with industry veterans
Phase 2: Market Size Estimation1
Top-down Assessment
- Estimation of total healthcare spending in the Philippines as a baseline (?1.56 trillion in 2024)
- Segmentation of fraud incidents by type (e.g., billing fraud, identity theft)
- Incorporation of government initiatives aimed at reducing healthcare fraud
Bottom-up Modeling
- Data collection from healthcare providers on reported fraud cases
- Cost analysis of fraud prevention measures implemented by hospitals
- Estimation of financial losses due to fraud based on industry benchmarks
Forecasting & Scenario Analysis
- Multi-variable regression analysis incorporating economic indicators and healthcare trends
- Scenario modeling based on potential regulatory changes and technological advancements
- Development of baseline, optimistic, and pessimistic forecasts through 2030
Phase 3: CATI Sample Composition1
| Scope Item/Segment | Sample Size | Target Respondent Profiles |
|---|---|---|
| Hospital Billing Fraud | 100 | Billing Managers, Compliance Officers |
| Insurance Fraud Investigations | 80 | Fraud Analysts, Claims Adjusters |
| Pharmaceutical Fraud Cases | 60 | Pharmacy Managers, Regulatory Affairs Specialists |
| Telemedicine Fraud Detection | 50 | Telehealth Coordinators, IT Security Managers |
| Healthcare Provider Compliance | 90 | Healthcare Administrators, Risk Management Officers |
Frequently Asked Questions
What is the current value of the Philippines Healthcare Fraud Analytics Market?
The Philippines Healthcare Fraud Analytics Market is valued at approximately USD 15 million, reflecting a significant investment in fraud detection and prevention technologies due to rising healthcare fraud incidents and regulatory compliance requirements.