About the Report
Base Year 2024Saudi Arabia Healthcare Reimbursement Market Overview
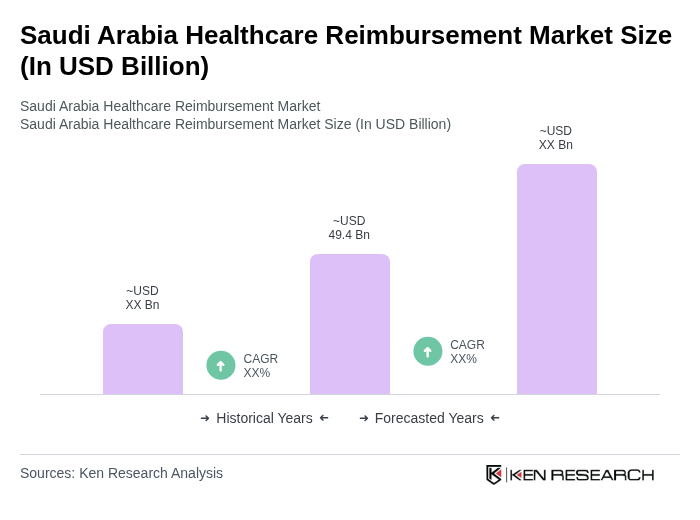
- The Saudi Arabia Healthcare Reimbursement Market is valued at USD 49.4 billion, based on a five-year historical analysis. This expansion is primarily driven by the increasing demand for healthcare services, sustained growth in overall healthcare expenditure, and the broadening of mandatory and voluntary health insurance coverage under the Council of Health Insurance framework. The government's commitment under Vision 2030 to enhance healthcare infrastructure, promote privatisation, and implement digital health and e-claims platforms such as the National Platform for Health and Insurance Exchange Services (NPHIES) has further strengthened reimbursement flows and market growth.
- Key cities such as Riyadh, Jeddah, and Dammam dominate the market due to their large populations, higher concentration of tertiary and specialist healthcare facilities, and dense employer and insured bases. Riyadh, as the capital, is the principal hub for healthcare services, insurance headquarters, and health clusters; Jeddah and the wider Western region benefit from strong commercial activity, pilgrimage-related healthcare demand, and extensive private hospital networks; while Dammam and the Eastern Province leverage industrial and oil-sector employment, population growth, and expanding private insurance penetration to drive reimbursement volumes.
- The health insurance framework is underpinned by the Cooperative Health Insurance Law issued by Royal Decree No. M/10 and implemented through the Council of Health Insurance regulations, which mandate that private?sector employers provide health insurance coverage for Saudi and expatriate employees and their eligible dependents. These binding rules define the Essential Benefits Package, minimum coverage standards, and electronic claims and reimbursement requirements, thereby expanding the insured population, standardizing benefits, and structurally increasing the demand for healthcare reimbursement services across the country.
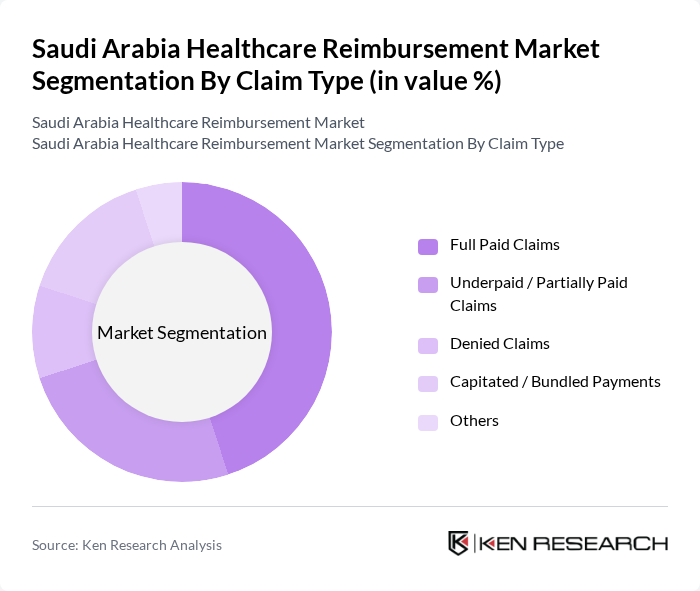
Saudi Arabia Healthcare Reimbursement Market Segmentation
By Claim Type:The claim type segmentation includes various categories that reflect the nature of healthcare reimbursements. The subsegments are Full Paid Claims, Underpaid / Partially Paid Claims, Denied Claims, Capitated / Bundled Payments, and Others. Full Paid Claims account for a substantial share of overall reimbursement value, supported by the growing number of insured lives, higher utilisation of inpatient and outpatient services, and improved electronic claims adjudication, although underpaid claims have emerged as a significant segment in specific areas such as medical devices reimbursement where they lead in revenue share.
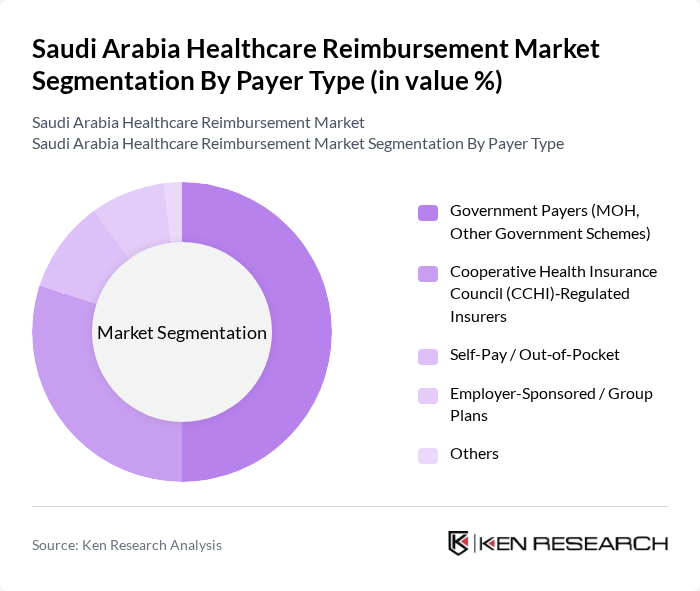
By Payer Type:The payer type segmentation encompasses various entities responsible for healthcare reimbursements. This includes Government Payers (MOH, Other Government Schemes), Cooperative Health Insurance Council (CCHI)?Regulated Insurers, Self-Pay / Out?of?Pocket, Employer-Sponsored / Group Plans, and Others. Government Payers continue to account for a major share of total health spending through the Ministry of Health and other public providers, while CCHI?regulated insurers represent the core of the cooperative health insurance market, which has grown to more than USD 10 billion and is increasingly shaped by employer?sponsored group policies and expanded dependent coverage.
Saudi Arabia Healthcare Reimbursement Market Competitive Landscape
The Saudi Arabia Healthcare Reimbursement Market is characterized by a dynamic mix of regional and international players. Leading participants such as Ministry of Health (MOH), Saudi Arabia, Council of Health Insurance (CHI), Saudi Arabia, Saudi National Unified Procurement Company (NUPCO), Bupa Arabia for Cooperative Insurance, The Company for Cooperative Insurance (Tawuniya), Arabian Shield Cooperative Insurance Company, Al Rajhi Company for Cooperative Insurance (Al Rajhi Takaful), Gulf Insurance Group – Saudi Arabia (GIG Saudi), Mediterranean and Gulf Cooperative Insurance and Reinsurance Company (Medgulf), Walaa Cooperative Insurance Company, Al-Etihad Cooperative Insurance Co., Aljazira Takaful Taawuni Company, Solidarity Saudi Takaful Company, AXA Cooperative Insurance Company, Malath Cooperative Insurance Co. contribute to innovation, geographic expansion, and service delivery in this space.
Saudi Arabia Healthcare Reimbursement Market Industry Analysis
Growth Drivers
- Increasing Healthcare Expenditure:Saudi Arabia's healthcare expenditure is projected to reach approximately SAR 200 billion (USD 53.3 billion) in future, reflecting a significant increase from SAR 189 billion in recent periods. This growth is driven by the government's commitment to enhancing healthcare services and infrastructure, as outlined in Vision 2030. The rising budget allocation supports the expansion of healthcare facilities and services, ultimately improving access to care and reimbursement processes for patients and providers alike.
- Rising Prevalence of Chronic Diseases:The prevalence of chronic diseases in Saudi Arabia is expected to rise, with diabetes cases projected to reach 4.3 million by future. This increase necessitates enhanced healthcare services and reimbursement mechanisms to manage these conditions effectively. The growing burden of chronic diseases drives demand for innovative treatment options and comprehensive care models, prompting healthcare providers to adapt their reimbursement strategies to accommodate the needs of this patient population.
- Government Initiatives for Healthcare Reforms:The Saudi government has initiated several reforms aimed at improving healthcare delivery, including the implementation of the National Health Insurance Law. This law is expected to cover over 70% of the population by future, significantly increasing access to healthcare services. These reforms are designed to streamline reimbursement processes, enhance service quality, and promote a more efficient healthcare system, ultimately benefiting both patients and providers.
Market Challenges
- Complex Regulatory Environment:The regulatory landscape in Saudi Arabia's healthcare reimbursement market is intricate, with multiple governing bodies involved. This complexity can lead to delays in reimbursement approvals and inconsistencies in policy implementation. For instance, the Ministry of Health and the Council of Cooperative Health Insurance both play critical roles, which can create confusion among healthcare providers regarding compliance and reimbursement procedures, ultimately affecting service delivery.
- Limited Awareness of Reimbursement Processes:Many healthcare providers in Saudi Arabia lack comprehensive knowledge of the reimbursement processes, which can hinder their ability to navigate the system effectively. A survey indicated that over 60% of healthcare professionals reported insufficient training on reimbursement protocols. This gap in understanding can lead to billing errors, delayed payments, and ultimately, reduced financial viability for healthcare institutions, impacting patient care quality.
Saudi Arabia Healthcare Reimbursement Market Future Outlook
The future of the Saudi Arabia healthcare reimbursement market appears promising, driven by ongoing digital transformation and a focus on patient-centered care. As telemedicine and digital health solutions gain traction, reimbursement models will likely evolve to accommodate these innovations. Additionally, the integration of artificial intelligence in reimbursement processes is expected to enhance efficiency and accuracy, ultimately improving patient outcomes and provider satisfaction. The emphasis on value-based care will further shape the landscape, aligning reimbursement with quality metrics and patient experiences.
Market Opportunities
- Growth of Telemedicine Services:The telemedicine market in Saudi Arabia is projected to reach SAR 1.5 billion (USD 400 million) by future, driven by increased demand for remote healthcare services. This growth presents an opportunity for reimbursement models to adapt, ensuring that telehealth services are adequately covered, thus enhancing access to care for patients in remote areas and improving overall healthcare delivery.
- Development of Value-Based Care Models:The shift towards value-based care is gaining momentum, with the government aiming to implement these models across various healthcare sectors. By future, it is anticipated that 30% of healthcare providers will adopt value-based reimbursement strategies. This transition offers opportunities for healthcare organizations to align their services with patient outcomes, fostering a more sustainable and efficient healthcare system.
Scope of the Report
| Segment | Sub-Segments |
|---|---|
| By Claim Type | Full Paid Claims Underpaid / Partially Paid Claims Denied Claims Capitated / Bundled Payments Others |
| By Payer Type | Government Payers (MOH, Other Government Schemes) Cooperative Health Insurance Council (CCHI)?Regulated Insurers Self-Pay / Out?of?Pocket Employer-Sponsored / Group Plans Others |
| By Healthcare Service Category | Inpatient Services Outpatient & Ambulatory Services Pharmacy & Prescription Drugs Medical Devices & Diagnostics Preventive & Wellness Services |
| By Provider Type | Public Hospitals & Medical Cities Private Hospitals Clinics & Polyclinics Diagnostic & Imaging Centers Home Healthcare & Long?Term Care Providers |
| By Region | Riyadh Region Makkah Region (including Jeddah) Eastern Province Northern & Western Regions Southern Regions |
| By Patient Demographics | Pediatric Patients Adult Patients Geriatric Patients Expatriate Population Special Needs & High?Risk Patients |
| By Technology Utilization in Reimbursement | Electronic Health Records (EHR)?Enabled Claims Telehealth & Virtual Care Claims Mobile Health Application?Based Claims Health Information Exchange (HIE) & e?Referral?Linked Claims AI / Analytics?Enabled Claims & Fraud Detection |
Key Target Audience
Investors and Venture Capitalist Firms
Government and Regulatory Bodies (e.g., Ministry of Health, Saudi Food and Drug Authority)
Healthcare Providers and Hospitals
Insurance Companies and Health Plans
Pharmaceutical Companies
Medical Device Manufacturers
Health Technology Companies
Healthcare Policy Makers
Players Mentioned in the Report:
Ministry of Health (MOH), Saudi Arabia
Council of Health Insurance (CHI), Saudi Arabia
Saudi National Unified Procurement Company (NUPCO)
Bupa Arabia for Cooperative Insurance
The Company for Cooperative Insurance (Tawuniya)
Arabian Shield Cooperative Insurance Company
Al Rajhi Company for Cooperative Insurance (Al Rajhi Takaful)
Gulf Insurance Group Saudi Arabia (GIG Saudi)
Mediterranean and Gulf Cooperative Insurance and Reinsurance Company (Medgulf)
Walaa Cooperative Insurance Company
Al-Etihad Cooperative Insurance Co.
Aljazira Takaful Taawuni Company
Solidarity Saudi Takaful Company
AXA Cooperative Insurance Company
Malath Cooperative Insurance Co.
Table of Contents
Market Assessment Phase
1. Executive Summary and Approach
2. Saudi Arabia Healthcare Reimbursement Market Overview
2.1 Key Insights and Strategic Recommendations
2.2 Saudi Arabia Healthcare Reimbursement Market Overview
2.3 Definition and Scope
2.4 Evolution of Market Ecosystem
2.5 Timeline of Key Regulatory Milestones
2.6 Value Chain & Stakeholder Mapping
2.7 Business Cycle Analysis
2.8 Policy & Incentive Landscape
3. Saudi Arabia Healthcare Reimbursement Market Analysis
3.1 Growth Drivers
3.1.1 Increasing healthcare expenditure
3.1.2 Rising prevalence of chronic diseases
3.1.3 Government initiatives for healthcare reforms
3.1.4 Expansion of private health insurance coverage
3.2 Market Challenges
3.2.1 Complex regulatory environment
3.2.2 Limited awareness of reimbursement processes
3.2.3 High dependency on government funding
3.2.4 Variability in reimbursement rates
3.3 Market Opportunities
3.3.1 Growth of telemedicine services
3.3.2 Development of value-based care models
3.3.3 Increased investment in healthcare technology
3.3.4 Expansion of outpatient services
3.4 Market Trends
3.4.1 Shift towards digital health solutions
3.4.2 Integration of AI in healthcare reimbursement
3.4.3 Focus on patient-centered care
3.4.4 Rise of personalized medicine
3.5 Government Regulation
3.5.1 Implementation of the National Health Insurance Law
3.5.2 Regulation of private health insurance providers
3.5.3 Standardization of reimbursement procedures
3.5.4 Monitoring of healthcare service quality
4. SWOT Analysis
5. Stakeholder Analysis
6. Porter's Five Forces Analysis
7. Saudi Arabia Healthcare Reimbursement Market Market Size, 2019-2024
7.1 By Value
7.2 By Volume
7.3 By Average Selling Price
8. Saudi Arabia Healthcare Reimbursement Market Segmentation
8.1 By Claim Type
8.1.1 Full Paid Claims
8.1.2 Underpaid / Partially Paid Claims
8.1.3 Denied Claims
8.1.4 Capitated / Bundled Payments
8.1.5 Others
8.2 By Payer Type
8.2.1 Government Payers (MOH, Other Government Schemes)
8.2.2 Cooperative Health Insurance Council (CCHI)?Regulated Insurers
8.2.3 Self-Pay / Out?of?Pocket
8.2.4 Employer-Sponsored / Group Plans
8.2.5 Others
8.3 By Healthcare Service Category
8.3.1 Inpatient Services
8.3.2 Outpatient & Ambulatory Services
8.3.3 Pharmacy & Prescription Drugs
8.3.4 Medical Devices & Diagnostics
8.3.5 Preventive & Wellness Services
8.4 By Provider Type
8.4.1 Public Hospitals & Medical Cities
8.4.2 Private Hospitals
8.4.3 Clinics & Polyclinics
8.4.4 Diagnostic & Imaging Centers
8.4.5 Home Healthcare & Long?Term Care Providers
8.5 By Region
8.5.1 Riyadh Region
8.5.2 Makkah Region (including Jeddah)
8.5.3 Eastern Province
8.5.4 Northern & Western Regions
8.5.5 Southern Regions
8.6 By Patient Demographics
8.6.1 Pediatric Patients
8.6.2 Adult Patients
8.6.3 Geriatric Patients
8.6.4 Expatriate Population
8.6.5 Special Needs & High?Risk Patients
8.7 By Technology Utilization in Reimbursement
8.7.1 Electronic Health Records (EHR)?Enabled Claims
8.7.2 Telehealth & Virtual Care Claims
8.7.3 Mobile Health Application?Based Claims
8.7.4 Health Information Exchange (HIE) & e?Referral?Linked Claims
8.7.5 AI / Analytics?Enabled Claims & Fraud Detection
9. Saudi Arabia Healthcare Reimbursement Market Competitive Analysis
9.1 Market Share of Key Players
9.2 Cross Comparison of Key Players
9.2.1 Company Name
9.2.2 Group Size (Large, Medium, or Small as per industry convention)
9.2.3 Gross Written Premiums from Health Insurance (SAR Million)
9.2.4 Healthcare Reimbursement Market Share (%)
9.2.5 Revenue Growth Rate from Health Segment (%)
9.2.6 Number of Covered Lives / Health Policies
9.2.7 Average Claim Processing Time (Days)
9.2.8 Claim Settlement Ratio (%)
9.2.9 Claim Rejection / Denial Rate (%)
9.2.10 Average Claim Size (SAR per Claim)
9.2.11 Loss Ratio for Health Line (%)
9.2.12 Digital Claims Adoption Rate (% of Claims Submitted Electronically)
9.2.13 Customer Satisfaction / NPS for Health Insurance
9.3 SWOT Analysis of Top Players
9.4 Pricing Analysis
9.5 Detailed Profile of Major Companies
9.5.1 Ministry of Health (MOH), Saudi Arabia
9.5.2 Council of Health Insurance (CHI), Saudi Arabia
9.5.3 Saudi National Unified Procurement Company (NUPCO)
9.5.4 Bupa Arabia for Cooperative Insurance
9.5.5 The Company for Cooperative Insurance (Tawuniya)
9.5.6 Arabian Shield Cooperative Insurance Company
9.5.7 Al Rajhi Company for Cooperative Insurance (Al Rajhi Takaful)
9.5.8 Gulf Insurance Group – Saudi Arabia (GIG Saudi)
9.5.9 Mediterranean and Gulf Cooperative Insurance and Reinsurance Company (Medgulf)
9.5.10 Walaa Cooperative Insurance Company
9.5.11 Al-Etihad Cooperative Insurance Co.
9.5.12 Aljazira Takaful Taawuni Company
9.5.13 Solidarity Saudi Takaful Company
9.5.14 AXA Cooperative Insurance Company
9.5.15 Malath Cooperative Insurance Co.
10. Saudi Arabia Healthcare Reimbursement Market End-User Analysis
10.1 Procurement Behavior of Key Ministries
10.1.1 Ministry of Health Procurement Strategies
10.1.2 Budget Allocation Trends
10.1.3 Contracting Processes
10.1.4 Evaluation Criteria for Vendors
10.2 Corporate Spend on Infrastructure & Energy
10.2.1 Investment in Healthcare Facilities
10.2.2 Spending on Medical Equipment
10.2.3 Budget for IT Infrastructure
10.2.4 Expenditure on Training and Development
10.3 Pain Point Analysis by End-User Category
10.3.1 Hospitals' Reimbursement Delays
10.3.2 Clinics' Administrative Burdens
10.3.3 Diagnostic Centers' Compliance Issues
10.3.4 Home Healthcare Providers' Funding Gaps
10.4 User Readiness for Adoption
10.4.1 Awareness of Reimbursement Processes
10.4.2 Training Needs for Staff
10.4.3 Technology Adoption Readiness
10.4.4 Financial Preparedness
10.5 Post-Deployment ROI and Use Case Expansion
10.5.1 Measurement of ROI Metrics
10.5.2 Case Studies of Successful Implementations
10.5.3 Expansion Opportunities in New Services
10.5.4 Long-term Sustainability Considerations
11. Saudi Arabia Healthcare Reimbursement Market Future Size, 2025-2030
11.1 By Value
11.2 By Volume
11.3 By Average Selling Price
Go-To-Market Strategy Phase
1. Whitespace Analysis + Business Model Canvas
1.1 Market Gaps Identification
1.2 Value Proposition Development
1.3 Revenue Streams Analysis
1.4 Cost Structure Evaluation
1.5 Key Partnerships Exploration
1.6 Customer Segmentation
1.7 Channels of Distribution
2. Marketing and Positioning Recommendations
2.1 Branding Strategies
2.2 Product USPs
2.3 Target Audience Identification
2.4 Communication Strategies
2.5 Digital Marketing Approaches
3. Distribution Plan
3.1 Urban Retail Strategies
3.2 Rural NGO Tie-ups
3.3 Online Distribution Channels
3.4 Partnerships with Healthcare Providers
4. Channel & Pricing Gaps
4.1 Underserved Routes
4.2 Pricing Bands Analysis
4.3 Competitor Pricing Strategies
4.4 Customer Willingness to Pay
5. Unmet Demand & Latent Needs
5.1 Category Gaps Identification
5.2 Consumer Segments Analysis
5.3 Emerging Trends Exploration
5.4 Future Needs Assessment
6. Customer Relationship
6.1 Loyalty Programs Development
6.2 After-sales Service Strategies
6.3 Customer Feedback Mechanisms
6.4 Community Engagement Initiatives
7. Value Proposition
7.1 Sustainability Initiatives
7.2 Integrated Supply Chains
7.3 Unique Selling Points
7.4 Customer-Centric Approaches
8. Key Activities
8.1 Regulatory Compliance
8.2 Branding Initiatives
8.3 Distribution Setup
8.4 Training and Development Programs
9. Entry Strategy Evaluation
9.1 Domestic Market Entry Strategy
9.1.1 Product Mix Considerations
9.1.2 Pricing Band Strategies
9.1.3 Packaging Innovations
9.2 Export Entry Strategy
9.2.1 Target Countries Identification
9.2.2 Compliance Roadmap Development
10. Entry Mode Assessment
10.1 Joint Ventures
10.2 Greenfield Investments
10.3 Mergers & Acquisitions
10.4 Distributor Model Evaluation
11. Capital and Timeline Estimation
11.1 Capital Requirements Analysis
11.2 Timelines for Implementation
12. Control vs Risk Trade-Off
12.1 Ownership Considerations
12.2 Partnerships Evaluation
13. Profitability Outlook
13.1 Breakeven Analysis
13.2 Long-term Sustainability Strategies
14. Potential Partner List
14.1 Distributors Identification
14.2 Joint Ventures Opportunities
14.3 Acquisition Targets
15. Execution Roadmap
15.1 Phased Plan for Market Entry
15.1.1 Market Setup
15.1.2 Market Entry
15.1.3 Growth Acceleration
15.1.4 Scale & Stabilize
15.2 Key Activities and Milestones
15.2.1 Milestone Planning
15.2.2 Activity Tracking
Research Methodology
Phase 1: Approach1
Desk Research
- Analysis of government healthcare expenditure reports and budget allocations
- Review of healthcare reimbursement policies from the Saudi Ministry of Health
- Examination of industry publications and white papers on healthcare financing trends
Primary Research
- Interviews with healthcare administrators and financial officers in hospitals
- Surveys with insurance providers regarding reimbursement models and practices
- Focus groups with healthcare professionals to understand reimbursement challenges
Validation & Triangulation
- Cross-validation of findings with data from international healthcare organizations
- Triangulation of reimbursement trends with patient outcome data and service utilization
- Sanity checks through expert panel reviews comprising healthcare economists
Phase 2: Market Size Estimation1
Top-down Assessment
- Estimation of total healthcare spending in Saudi Arabia as a baseline
- Segmentation of the market by reimbursement types: public vs. private
- Incorporation of demographic trends and disease prevalence rates
Bottom-up Modeling
- Collection of data on reimbursement rates from major healthcare providers
- Analysis of patient volume and service utilization across different healthcare sectors
- Cost analysis based on treatment types and associated reimbursement levels
Forecasting & Scenario Analysis
- Multi-factor regression analysis incorporating economic indicators and healthcare reforms
- Scenario modeling based on potential changes in insurance coverage and policy shifts
- Baseline, optimistic, and pessimistic forecasts through 2030
Phase 3: CATI Sample Composition1
| Scope Item/Segment | Sample Size | Target Respondent Profiles |
|---|---|---|
| Public Healthcare Facilities | 100 | Hospital Administrators, Financial Officers |
| Private Insurance Providers | 80 | Claims Managers, Underwriters |
| Pharmaceutical Reimbursement Processes | 70 | Pharmacy Directors, Reimbursement Specialists |
| Healthcare Technology Adoption | 60 | IT Managers, Health Informatics Specialists |
| Patient Experience and Satisfaction | 90 | Patient Advocates, Healthcare Quality Managers |
Frequently Asked Questions
What is the current value of the Saudi Arabia Healthcare Reimbursement Market?
The Saudi Arabia Healthcare Reimbursement Market is valued at approximately USD 49.4 billion, reflecting a significant growth driven by increased healthcare service demand and expanded health insurance coverage under the Council of Health Insurance framework.