Region:Global
Author(s):Dev
Product Code:KRAE0243
Pages:85
Published On:December 2025
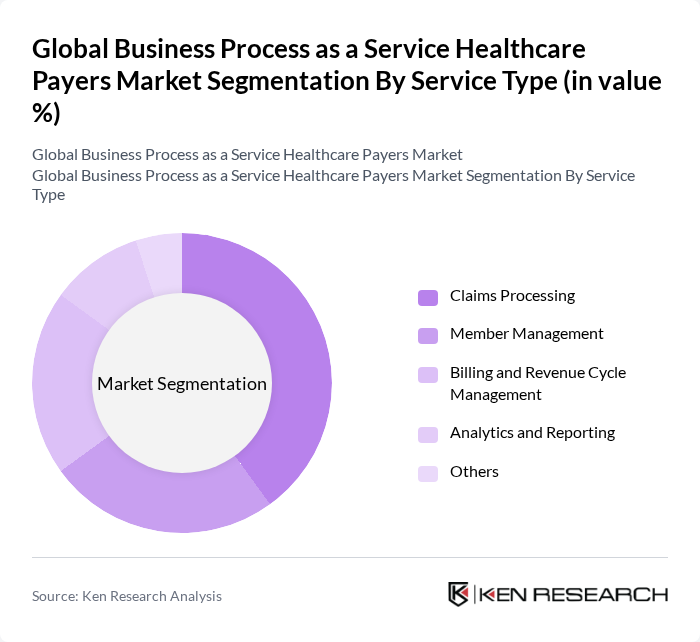
By Service Type:The service type segmentation of the market includes various critical functions that healthcare payers require to enhance their operational efficiency. Claims processing is the most significant segment, driven by the increasing volume of claims and the need for accuracy and speed in processing. Member management and billing and revenue cycle management are also crucial, as they directly impact customer satisfaction and revenue generation. Analytics and reporting services are gaining traction as payers seek to leverage data for better decision-making and compliance.
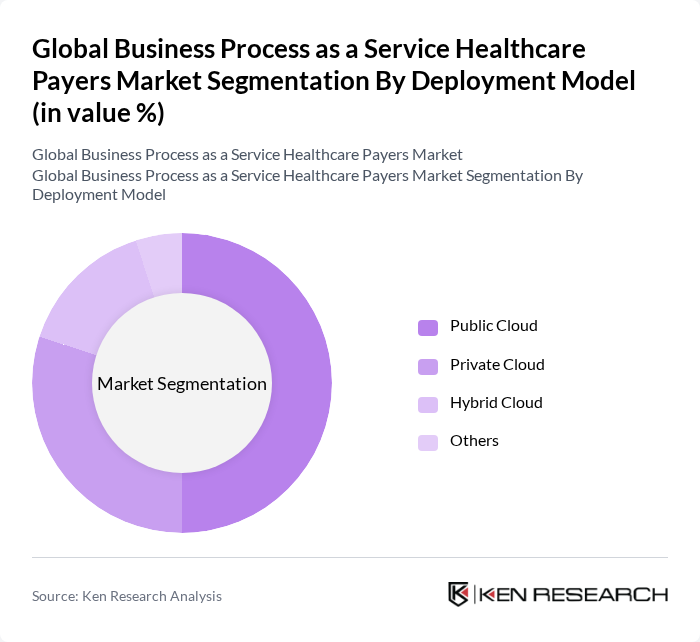
By Deployment Model:The deployment model segmentation highlights the various ways BPaaS solutions are delivered to healthcare payers. Public cloud solutions are leading the market due to their cost-effectiveness and scalability, allowing payers to quickly adapt to changing demands. Private cloud solutions are preferred by organizations with stringent data security requirements, while hybrid cloud models are gaining popularity as they offer a balance between flexibility and control. The "Others" category includes on-premise solutions, which are less common but still relevant for certain organizations.
The Global Business Process as a Service Healthcare Payers Market is characterized by a dynamic mix of regional and international players. Leading participants such as Optum, Cognizant Technology Solutions, Accenture, Cerner Corporation, Change Healthcare, McKesson Corporation, Allscripts Healthcare Solutions, DXC Technology, IBM Watson Health, R1 RCM, eCatalyst Healthcare Solutions, Medidata Solutions, NextGen Healthcare, Philips Healthcare, Siemens Healthineers contribute to innovation, geographic expansion, and service delivery in this space.
The future of the BPaaS healthcare payers market is poised for significant transformation, driven by technological advancements and evolving consumer expectations. As healthcare organizations increasingly prioritize digital transformation, the demand for integrated, cloud-based solutions will rise. Additionally, the focus on value-based care models will encourage payers to adopt innovative approaches that enhance patient outcomes while controlling costs. This shift will likely lead to greater collaboration between payers and technology providers, fostering a more efficient healthcare ecosystem.
| Segment | Sub-Segments |
|---|---|
| By Service Type | Claims Processing Member Management Billing and Revenue Cycle Management Analytics and Reporting Others |
| By Deployment Model | Public Cloud Private Cloud Hybrid Cloud Others |
| By Customer Size | Small Enterprises Medium Enterprises Large Enterprises Others |
| By Geographic Presence | North America Europe Asia-Pacific Latin America Middle East & Africa |
| By End-User Type | Insurance Companies Healthcare Providers Third-Party Administrators Others |
| By Technology Used | Artificial Intelligence Machine Learning Blockchain Others |
| By Service Delivery Model | On-Premise Off-Premise Others |
| Scope Item/Segment | Sample Size | Target Respondent Profiles |
|---|---|---|
| Claims Processing Solutions | 150 | Claims Managers, IT Directors |
| Data Analytics Services | 100 | Data Analysts, Business Intelligence Managers |
| Patient Engagement Platforms | 80 | Patient Experience Officers, Marketing Managers |
| Fraud Detection Systems | 70 | Compliance Officers, Risk Management Directors |
| Telehealth Integration Services | 90 | Telehealth Coordinators, IT Support Managers |
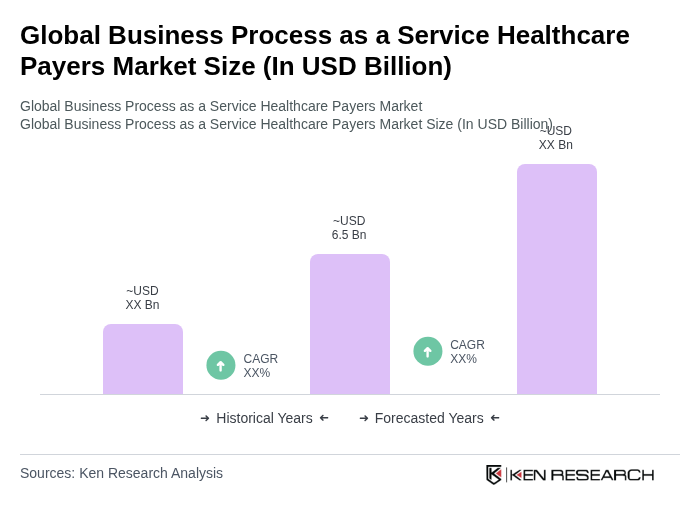
The Global Business Process as a Service Healthcare Payers Market is valued at approximately USD 6.5 billion, reflecting a significant demand for operational efficiency and cost reduction among healthcare payers.