Region:Middle East
Author(s):Dev
Product Code:KRAC3452
Pages:98
Published On:October 2025
 Healthcare Payer Market.png)
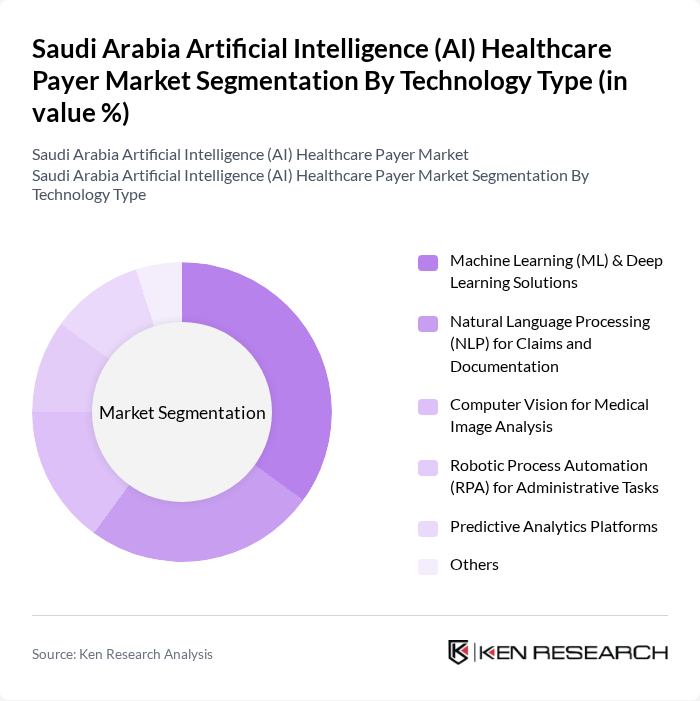
By Technology Type:The technology type segmentation includes various AI technologies utilized in the healthcare payer market. The leading sub-segment isMachine Learning (ML) & Deep Learning Solutions, widely adopted for predictive analytics, risk scoring, and automating decision-making processes.Natural Language Processing (NLP) for Claims and Documentationis gaining traction, streamlining administrative tasks and enhancing efficiency in claims review and medical coding.Computer Visionis increasingly used for medical image analysis and document verification, whileRobotic Process Automation (RPA)automates repetitive administrative tasks such as billing and eligibility checks.Predictive Analytics Platformssupport population health management and cost forecasting. Other emerging technologies include AI-powered chatbots and virtual assistants for member engagement .
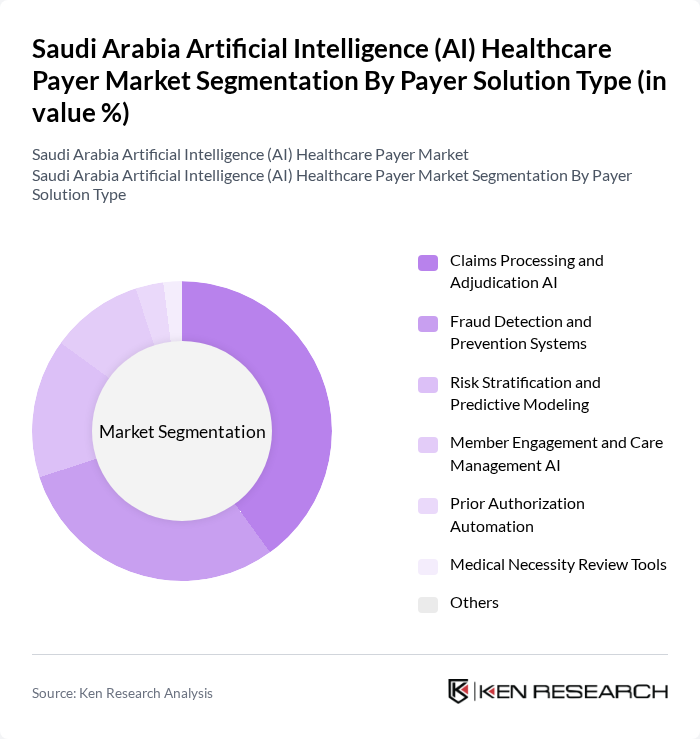
By Payer Solution Type:The payer solution type segmentation highlights various AI-driven solutions that enhance operational efficiency and reduce costs for healthcare payers.Claims Processing and Adjudication AIis the leading sub-segment, automating and streamlining the claims process to reduce turnaround times and errors.Fraud Detection and Prevention Systemsare critical, leveraging AI algorithms to identify suspicious patterns and prevent fraudulent claims.Risk Stratification and Predictive Modelingsupport proactive member management and cost control.Member Engagement and Care Management AIsolutions use chatbots and personalized outreach to improve member satisfaction and retention.Prior Authorization AutomationandMedical Necessity Review Toolsare emerging, enabling faster approvals and compliance checks .
The Saudi Arabia Artificial Intelligence (AI) Healthcare Payer Market is characterized by a dynamic mix of regional and international players. Leading participants such as IBM Watson Health, Optum (UnitedHealth Group), Change Healthcare, Cerner Corporation, Allscripts Healthcare Solutions, McKesson Corporation, Veradigm (Allscripts subsidiary), Health Catalyst, Nuance Communications (Microsoft subsidiary), Siemens Healthineers, GE Healthcare, M42 Digital Health (Abu Dhabi-based, regional player), Philips Healthcare, Medtronic, eClinicalWorks contribute to innovation, geographic expansion, and service delivery in this space.
The future of the AI healthcare payer market in Saudi Arabia appears promising, driven by ongoing advancements in technology and increasing government support. As healthcare payers continue to embrace AI solutions, we can expect enhanced operational efficiencies and improved patient outcomes. The integration of AI in telemedicine and remote monitoring will likely expand, providing real-time analytics and personalized care. Furthermore, strategic collaborations with global tech leaders will foster innovation, ensuring that the market remains competitive and responsive to evolving healthcare needs.
| Segment | Sub-Segments |
|---|---|
| By Technology Type | Machine Learning (ML) & Deep Learning Solutions Natural Language Processing (NLP) for Claims and Documentation Computer Vision for Medical Image Analysis Robotic Process Automation (RPA) for Administrative Tasks Predictive Analytics Platforms Others |
| By Payer Solution Type | Claims Processing and Adjudication AI Fraud Detection and Prevention Systems Risk Stratification and Predictive Modeling Member Engagement and Care Management AI Prior Authorization Automation Medical Necessity Review Tools Others |
| By End-User | Insurance Companies and Health Plans Government Health Agencies (Ministry of Health) Third-Party Administrators (TPAs) Healthcare Providers (Hospitals and Clinics) Employers and Corporate Health Benefit Programs Others |
| By Application | Claims Management and Processing Fraud, Waste, and Abuse Detection Risk Assessment and Member Stratification Utilization Management and Authorization Member Engagement and Retention Provider Network Optimization Others |
| By Deployment Model | Cloud-Based Solutions On-Premise Solutions Hybrid Deployment SaaS Platforms Others |
| By Pricing Model | Subscription-Based (SaaS) Per-Transaction or Per-Claim Pricing Fixed Licensing Fees Value-Based/Outcome-Based Pricing Others |
| By Customer Size | Large Payers (>500,000 members) Mid-Size Payers (100,000-500,000 members) Small Payers (<100,000 members) Government and Public Healthcare Systems Others |
| By Region | Central Region (Riyadh) Eastern Region (Dammam, Khobar) Western Region (Jeddah, Mecca) Southern Region (Abha) Northern Region |
| Scope Item/Segment | Sample Size | Target Respondent Profiles |
|---|---|---|
| Public Healthcare Payers | 50 | Healthcare Administrators, Policy Makers |
| Private Health Insurance Providers | 40 | Insurance Executives, Product Managers |
| AI Technology Vendors in Healthcare | 30 | Product Development Leads, Sales Directors |
| Healthcare Professionals Using AI | 60 | Doctors, Nurses, IT Specialists |
| Regulatory Bodies and Health Authorities | 40 | Regulatory Officers, Compliance Managers |
The Saudi Arabia Artificial Intelligence (AI) Healthcare Payer Market is valued at approximately USD 210 million, reflecting significant growth driven by the adoption of AI technologies aimed at enhancing operational efficiency and patient care.