About the Report
Base Year 2024Australia Healthcare Payer Services Market Overview
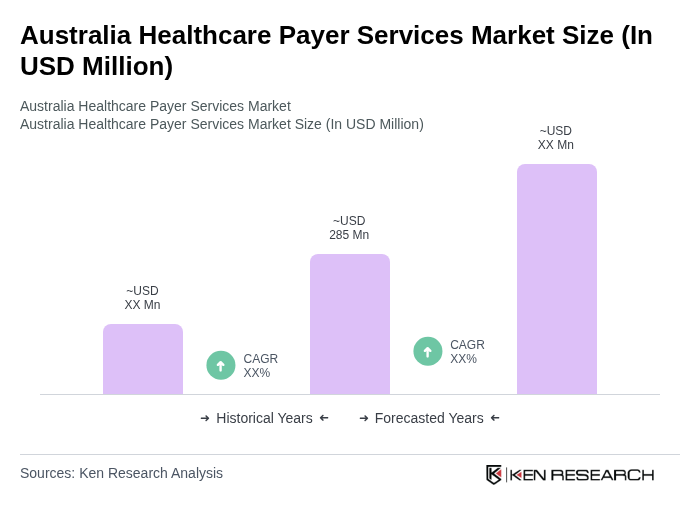
- The Australia Healthcare Payer Services Market is valued at USD 285 million, based on a five-year historical analysis. This growth is primarily driven by the increasing demand for healthcare services, technological advancements in healthcare IT, rising prevalence of chronic diseases, growing penetration of private health insurance, and expansion of telehealth services, which have become essential in the current healthcare landscape.
- Key players in this market include major cities such as Sydney, Melbourne, and Brisbane, which dominate due to their robust healthcare infrastructure, high population density, and significant investment in healthcare technology. These cities are home to numerous healthcare facilities and insurance companies, making them central hubs for healthcare payer services in Australia.
- The Private Health Insurance (National Joint Policy Committee – Information Provision) Rule 2019, issued by the Private Health Insurance Ombudsman, mandates private health insurers to provide standardized product information including out-of-pocket costs, coverage details, and benefit entitlements through the government’s privatehealth.gov.au comparison website, with compliance requiring annual product disclosure updates and adherence to specified data formats for consumer transparency.
Australia Healthcare Payer Services Market Segmentation
By Service Type:
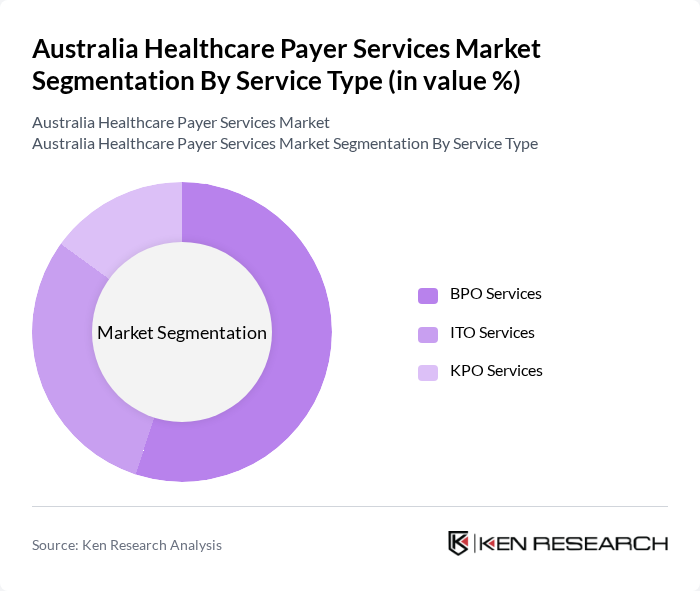
The service type segmentation includes BPO Services, ITO Services, and KPO Services. Among these, ITO Services dominate the market due to the increasing need for efficient claims processing and customer service management. The demand for outsourcing these functions allows healthcare payers to focus on core activities while improving operational efficiency. BPO Services are also gaining traction as healthcare organizations seek to leverage technology for better data management and analytics. KPO Services, while smaller in market share, are growing as payers look for specialized knowledge and expertise in areas like clinical research and data analysis.
By Application:
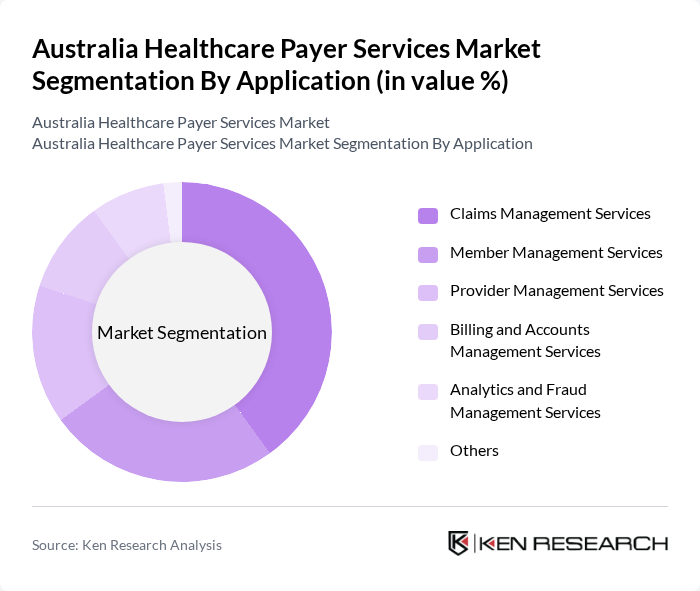
The application segmentation includes Claims Management Services, Member Management Services, Provider Management Services, Billing and Accounts Management Services, Analytics and Fraud Management Services, and Others. Claims Management Services lead the market as they are critical for ensuring timely reimbursements and managing healthcare costs effectively. Member Management Services are also significant, driven by the need for personalized care and engagement strategies. The increasing focus on analytics and fraud management is pushing the demand for these services, as payers seek to enhance operational efficiency and reduce fraudulent activities.
Australia Healthcare Payer Services Market Competitive Landscape
The Australia Healthcare Payer Services Market is characterized by a dynamic mix of regional and international players. Leading participants such as Medibank Private Limited, Bupa Australia, NIB Health Funds, HCF Life Insurance, Australian Unity, CBHS Health Fund, Teachers Health Fund, Frank Health Insurance, ahm Health Insurance, DVA Health, Qantas Health, Health.com.au, St. Lukes Health, GMHBA, Peoplecare Health Insurance contribute to innovation, geographic expansion, and service delivery in this space.
Australia Healthcare Payer Services Market Industry Analysis
Growth Drivers
- Increasing Demand for Healthcare Services:The Australian healthcare sector is experiencing a significant surge in demand, driven by an aging population projected to reach 9 million in the future. This demographic shift is accompanied by a rise in chronic diseases, with 50% of Australians aged 65 and older living with multiple health conditions. Consequently, healthcare payer services are expanding to accommodate this growing need, supported by government expenditure on health, which is expected to exceed AUD 120 billion in the future.
- Technological Advancements in Healthcare:The integration of advanced technologies in healthcare is revolutionizing payer services in Australia. In future, the Australian government is investing AUD 2 billion in digital health initiatives, including electronic health records and telehealth platforms. This investment is expected to enhance service delivery and patient engagement, leading to improved health outcomes. Moreover, the adoption of AI and machine learning in claims processing is projected to reduce administrative costs by 25%, further driving market growth.
- Government Initiatives and Funding:The Australian government is actively promoting healthcare payer services through various initiatives and funding programs. In future, the government plans to allocate AUD 3 billion to support health insurance reforms aimed at increasing accessibility and affordability. Additionally, the introduction of the Health Care Homes initiative is expected to enhance chronic disease management, thereby increasing the demand for payer services. These initiatives are crucial in shaping a sustainable healthcare system that meets the needs of all Australians.
Market Challenges
- Regulatory Compliance Issues:Navigating the complex regulatory landscape poses significant challenges for healthcare payer services in Australia. Compliance with the National Health Act and the Private Health Insurance Act requires substantial resources and expertise. In future, the Australian Competition and Consumer Commission (ACCC) is expected to increase scrutiny on pricing practices, which may lead to heightened compliance costs for payers. This regulatory burden can hinder innovation and operational efficiency within the sector.
- Data Security and Privacy Concerns:As healthcare payer services increasingly rely on digital platforms, data security and privacy have become paramount concerns. In future, the Australian Cyber Security Centre reported a 35% increase in cyber incidents targeting healthcare organizations. The potential for data breaches not only jeopardizes patient trust but also incurs significant financial penalties under the Privacy Act. Addressing these security challenges is essential for maintaining the integrity of healthcare payer services and protecting sensitive patient information.
Australia Healthcare Payer Services Market Future Outlook
The future of the Australia healthcare payer services market is poised for transformation, driven by technological advancements and evolving consumer expectations. The shift towards value-based care is expected to redefine service delivery, emphasizing patient outcomes over volume. Additionally, the integration of personalized medicine will enhance treatment efficacy, catering to individual patient needs. As these trends unfold, payer services will increasingly focus on innovative solutions that improve accessibility and affordability, ensuring a sustainable healthcare ecosystem for all Australians.
Market Opportunities
- Expansion of Telehealth Services:The telehealth sector in Australia is projected to grow significantly, with an estimated 20 million telehealth consultations expected in future. This expansion presents a lucrative opportunity for healthcare payers to enhance service delivery and patient engagement, ultimately improving health outcomes while reducing costs associated with in-person visits.
- Partnerships with Technology Providers:Collaborations with technology firms are becoming increasingly vital for healthcare payer services. In future, partnerships with tech providers are expected to drive innovation in claims processing and patient management systems. These alliances can enhance operational efficiency and improve service offerings, positioning payers to better meet the demands of a rapidly evolving healthcare landscape.
Scope of the Report
| Segment | Sub-Segments |
|---|---|
| By Service Type | BPO Services ITO Services KPO Services |
| By Application | Claims Management Services Member Management Services Provider Management Services Billing and Accounts Management Services Analytics and Fraud Management Services Others |
| By End-User | Private Payers Public Payers |
Key Target Audience
Investors and Venture Capitalist Firms
Government and Regulatory Bodies (e.g., Australian Department of Health, Australian Competition and Consumer Commission)
Health Insurance Providers
Pharmaceutical Benefit Managers
Healthcare Technology Companies
Healthcare Service Providers
Industry Associations (e.g., Private Health Insurance Administration Council)
Financial Institutions and Investment Banks
Players Mentioned in the Report:
Medibank Private Limited
Bupa Australia
NIB Health Funds
HCF Life Insurance
Australian Unity
CBHS Health Fund
Teachers Health Fund
Frank Health Insurance
ahm Health Insurance
DVA Health
Qantas Health
Health.com.au
St. Lukes Health
GMHBA
Peoplecare Health Insurance
Table of Contents
Market Assessment Phase
1. Executive Summary and Approach
2. Australia Healthcare Payer Services Market Overview
2.1 Key Insights and Strategic Recommendations
2.2 Australia Healthcare Payer Services Market Overview
2.3 Definition and Scope
2.4 Evolution of Market Ecosystem
2.5 Timeline of Key Regulatory Milestones
2.6 Value Chain & Stakeholder Mapping
2.7 Business Cycle Analysis
2.8 Policy & Incentive Landscape
3. Australia Healthcare Payer Services Market Analysis
3.1 Growth Drivers
3.1.1 Increasing Demand for Healthcare Services
3.1.2 Technological Advancements in Healthcare
3.1.3 Rising Healthcare Costs
3.1.4 Government Initiatives and Funding
3.2 Market Challenges
3.2.1 Regulatory Compliance Issues
3.2.2 Data Security and Privacy Concerns
3.2.3 Competition from Emerging Players
3.2.4 Integration of New Technologies
3.3 Market Opportunities
3.3.1 Expansion of Telehealth Services
3.3.2 Growth in Health Insurance Coverage
3.3.3 Partnerships with Technology Providers
3.3.4 Increasing Focus on Preventive Care
3.4 Market Trends
3.4.1 Shift Towards Value-Based Care
3.4.2 Rise of Personalized Medicine
3.4.3 Integration of AI and Machine Learning
3.4.4 Emphasis on Patient-Centric Services
3.5 Government Regulation
3.5.1 National Health Reform Initiatives
3.5.2 Privacy and Data Protection Laws
3.5.3 Licensing and Accreditation Requirements
3.5.4 Funding and Subsidy Programs
4. SWOT Analysis
5. Stakeholder Analysis
6. Porter's Five Forces Analysis
7. Australia Healthcare Payer Services Market Market Size, 2019-2024
7.1 By Value
7.2 By Volume
7.3 By Average Selling Price
8. Australia Healthcare Payer Services Market Segmentation
8.1 By Service Type
8.1.1 BPO Services
8.1.2 ITO Services
8.1.3 KPO Services
8.2 By Application
8.2.1 Claims Management Services
8.2.2 Member Management Services
8.2.3 Provider Management Services
8.2.4 Billing and Accounts Management Services
8.2.5 Analytics and Fraud Management Services
8.2.6 Others
8.3 By End-User
8.3.1 Private Payers
8.3.2 Public Payers
9. Australia Healthcare Payer Services Market Competitive Analysis
9.1 Market Share of Key Players
9.2 Cross Comparison of Key Players
9.2.1 Company Name
9.2.2 Market Share (%)
9.2.3 Revenue Growth Rate (CAGR)
9.2.4 EBITDA Margin
9.2.5 Claims Processing Efficiency (Turnaround Time)
9.2.6 Customer Retention Rate
9.2.7 Net Promoter Score (NPS)
9.2.8 Medical Loss Ratio (MLR)
9.2.9 Return on Equity (ROE)
9.2.10 Total Addressable Market Penetration
9.3 SWOT Analysis of Top Players
9.4 Pricing Analysis
9.5 Detailed Profile of Major Companies
9.5.1 Medibank Private Limited
9.5.2 Bupa Australia
9.5.3 NIB Health Funds
9.5.4 HCF Life Insurance
9.5.5 Australian Unity
9.5.6 CBHS Health Fund
9.5.7 Teachers Health Fund
9.5.8 Frank Health Insurance
9.5.9 ahm Health Insurance
9.5.10 DVA Health
9.5.11 Qantas Health
9.5.12 Health.com.au
9.5.13 St. Lukes Health
9.5.14 GMHBA
9.5.15 Peoplecare Health Insurance
10. Australia Healthcare Payer Services Market End-User Analysis
10.1 Procurement Behavior of Key Ministries
10.1.1 Budget Allocation Trends
10.1.2 Decision-Making Processes
10.1.3 Preferred Service Providers
10.1.4 Contracting Practices
10.2 Corporate Spend on Infrastructure & Energy
10.2.1 Investment Priorities
10.2.2 Spending Patterns
10.2.3 Cost Management Strategies
10.2.4 Future Spending Projections
10.3 Pain Point Analysis by End-User Category
10.3.1 Individual Policyholders
10.3.2 Corporates
10.3.3 Government Entities
10.3.4 Others
10.4 User Readiness for Adoption
10.4.1 Awareness Levels
10.4.2 Training Needs
10.4.3 Technology Acceptance
10.4.4 Support Requirements
10.5 Post-Deployment ROI and Use Case Expansion
10.5.1 Measurement of Success
10.5.2 Case Studies
10.5.3 Future Use Cases
10.5.4 Feedback Mechanisms
11. Australia Healthcare Payer Services Market Future Size, 2025-2030
11.1 By Value
11.2 By Volume
11.3 By Average Selling Price
Go-To-Market Strategy Phase
1. Whitespace Analysis + Business Model Canvas
1.1 Market Gaps Identification
1.2 Business Model Framework
2. Marketing and Positioning Recommendations
2.1 Branding Strategies
2.2 Product USPs
3. Distribution Plan
3.1 Urban Retail Strategies
3.2 Rural NGO Tie-Ups
4. Channel & Pricing Gaps
4.1 Underserved Routes
4.2 Pricing Bands
5. Unmet Demand & Latent Needs
5.1 Category Gaps
5.2 Consumer Segments
6. Customer Relationship
6.1 Loyalty Programs
6.2 After-Sales Service
7. Value Proposition
7.1 Sustainability
7.2 Integrated Supply Chains
8. Key Activities
8.1 Regulatory Compliance
8.2 Branding
8.3 Distribution Setup
9. Entry Strategy Evaluation
9.1 Domestic Market Entry Strategy
9.1.1 Product Mix
9.1.2 Pricing Band
9.1.3 Packaging
9.2 Export Entry Strategy
9.2.1 Target Countries
9.2.2 Compliance Roadmap
10. Entry Mode Assessment
10.1 Joint Ventures
10.2 Greenfield Investments
10.3 Mergers & Acquisitions
10.4 Distributor Model
11. Capital and Timeline Estimation
11.1 Capital Requirements
11.2 Timelines
12. Control vs Risk Trade-Off
12.1 Ownership vs Partnerships
13. Profitability Outlook
13.1 Breakeven Analysis
13.2 Long-Term Sustainability
14. Potential Partner List
14.1 Distributors
14.2 Joint Ventures
14.3 Acquisition Targets
15. Execution Roadmap
15.1 Phased Plan for Market Entry
15.1.1 Market Setup
15.1.2 Market Entry
15.1.3 Growth Acceleration
15.1.4 Scale & Stabilize
15.2 Key Activities and Milestones
15.2.1 Milestone Planning
15.2.2 Activity Tracking
Research Methodology
Phase 1: Approach1
Desk Research
- Analysis of government healthcare expenditure reports and statistics from the Australian Institute of Health and Welfare
- Review of industry publications and white papers from healthcare consulting firms
- Examination of market trends and forecasts from healthcare payer service associations
Primary Research
- Interviews with executives from major health insurance companies operating in Australia
- Surveys targeting healthcare policy experts and analysts
- Focus groups with healthcare providers to understand payer-provider dynamics
Validation & Triangulation
- Cross-validation of findings through multiple data sources, including government and private sector reports
- Triangulation of qualitative insights from interviews with quantitative data from surveys
- Sanity checks conducted through expert panel reviews comprising industry veterans
Phase 2: Market Size Estimation1
Top-down Assessment
- Estimation of total healthcare spending in Australia as a baseline for payer services
- Segmentation of the market by payer type, including private health insurers and government programs
- Incorporation of demographic trends and aging population statistics to project future growth
Bottom-up Modeling
- Analysis of premium revenue data from leading health insurance providers
- Estimation of service utilization rates based on historical claims data
- Calculation of average costs per service type to derive total market value
Forecasting & Scenario Analysis
- Multi-variable regression analysis incorporating economic indicators and healthcare policy changes
- Scenario modeling based on potential shifts in regulatory frameworks and consumer behavior
- Development of baseline, optimistic, and pessimistic forecasts through 2030
Phase 3: CATI Sample Composition1
| Scope Item/Segment | Sample Size | Target Respondent Profiles |
|---|---|---|
| Private Health Insurance Providers | 45 | CEOs, CFOs, and Strategy Directors |
| Government Healthcare Programs | 40 | Policy Makers, Program Managers |
| Healthcare Technology Solutions | 42 | IT Directors, Product Managers |
| Healthcare Provider Networks | 43 | Network Managers, Clinical Directors |
| Consumer Insights on Health Insurance | 48 | Policyholders, Healthcare Consumers |
Frequently Asked Questions
What is the current value of the Australia Healthcare Payer Services Market?
The Australia Healthcare Payer Services Market is valued at approximately USD 285 million, reflecting a five-year historical analysis. This growth is driven by increasing healthcare demands, technological advancements, and the rise of chronic diseases among the population.