Region:Middle East
Author(s):Geetanshi
Product Code:KRAB1140
Pages:84
Published On:January 2026
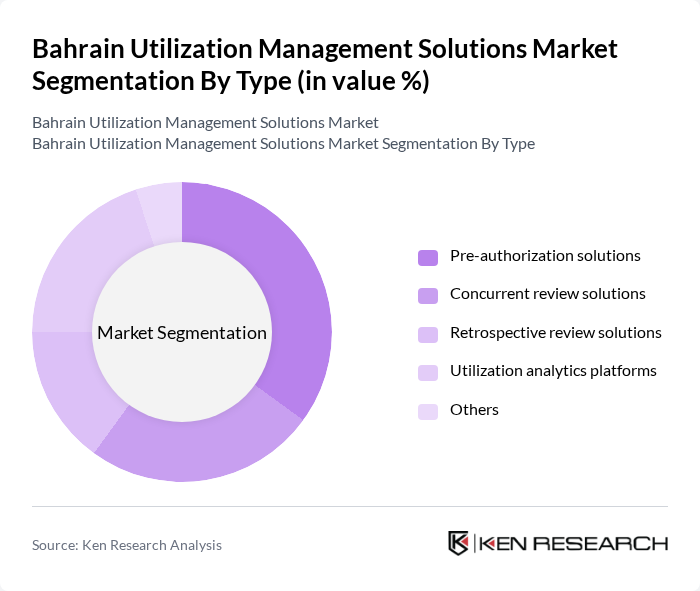
By Type:The market is segmented into various types of utilization management solutions, including pre-authorization solutions, concurrent review solutions, retrospective review solutions, utilization analytics platforms, and others. Among these, pre-authorization solutions are currently leading the market due to their critical role in managing healthcare costs and ensuring that patients receive necessary services without unnecessary delays. The increasing focus on cost containment and efficiency in healthcare delivery has driven the adoption of these solutions.
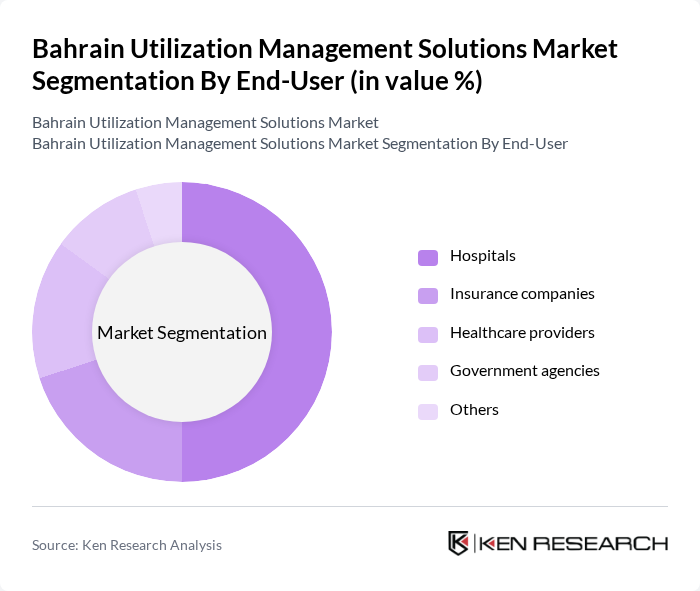
By End-User:The end-user segmentation includes hospitals, insurance companies, healthcare providers, government agencies, and others. Hospitals are the dominant end-user segment, driven by the need for efficient patient management and resource allocation. The increasing pressure on hospitals to optimize their operations and reduce costs has led to a higher adoption of utilization management solutions, making them a critical component in hospital management strategies.
The Bahrain Utilization Management Solutions Market is characterized by a dynamic mix of regional and international players. Leading participants such as Cerner Corporation, OptumHealth, McKesson Corporation, Allscripts Healthcare Solutions, eClinicalWorks, Medtronic, Philips Healthcare, IBM Watson Health, Change Healthcare, NextGen Healthcare, Greenway Health, Athenahealth, Siemens Healthineers, GE Healthcare, and Oracle Health Sciences contribute to innovation, geographic expansion, and service delivery in this space.
The future of the Bahrain utilization management solutions market appears promising, driven by the integration of advanced technologies such as AI and machine learning in healthcare. The rollout of the Sehati health insurance program in early future is expected to further stimulate demand for utilization management solutions, as healthcare providers will need to optimize their operations to manage insurance claims effectively. Additionally, the ongoing digital transformation initiatives will likely enhance the adoption of innovative healthcare solutions, improving overall efficiency and patient care outcomes.
| Segment | Sub-Segments |
|---|---|
| By Type | Pre-authorization solutions Concurrent review solutions Retrospective review solutions Utilization analytics platforms Others |
| By End-User | Hospitals Insurance companies Healthcare providers Government agencies Others |
| By Region | Northern Governorate Southern Governorate Capital Governorate Muharraq Governorate |
| By Technology | Cloud-based solutions On-premise solutions Hybrid solutions Others |
| By Application | Inpatient management Outpatient management Emergency care management Others |
| By Investment Source | Private investments Government funding Public-private partnerships Others |
| By Policy Support | Government subsidies Tax incentives Regulatory support Others |
| Scope Item/Segment | Sample Size | Target Respondent Profiles |
|---|---|---|
| Hospital Utilization Management | 100 | Healthcare Administrators, Utilization Review Managers |
| Insurance Provider Practices | 80 | Claims Managers, Medical Directors |
| Outpatient Services Management | 70 | Practice Managers, Clinical Coordinators |
| Telehealth Utilization Strategies | 60 | Telehealth Program Directors, IT Managers |
| Healthcare Policy Impact Assessment | 90 | Healthcare Policy Analysts, Economists |
The Bahrain Utilization Management Solutions Market is valued at approximately USD 2.80 billion, reflecting significant growth driven by the digitization of healthcare services and the demand for AI-enabled care optimization.